The delta wave is a type of brainwave that is seen in deep sleep, during the first stage of NREM. It occurs when the brain is in a very relaxed state and shows that the person is healthy and has good sleep quality.
The delta wave is an EEG recording pattern that shows up as a slow, high amplitude signal on an electroencephalogram (EEG). Delta waves are seen during deep non-REM sleep and are most pronounced in children under the age of 6 years old.
Delta waves are a type of brainwave recorded by electroencephalography (EEG) that show up as high amplitude signals on an EEG. They occur in deep non-rapid eye movement (NREM) sleep and represent a state of deep relaxation and restorative function. Delta waves have also been associated with increased learning ability when people experience them during sleep, according to researchers at Harvard University Medical School in Massachusetts.
The delta wave, which is a type of slow wave, is associated with deep sleep. This rhythm is often seen during the first stage of non-rapid eye movement sleep (NREM). Delta waves are an indication that the brain and body are relaxed and at rest.
The delta wave represents the deepest level of sleep. It is not uncommon for people to be awakened by a loud noise during this stage of sleep. If you are awakened during this time, it may take several minutes to return to full consciousness. Your body temperature drops significantly, and your heart rate slows down significantly as well. The body uses this time to heal itself and restore energy levels after having been awake all day long.
What does a delta wave mean on ECG?

A delta wave is a type of abnormal heart rhythm. It’s a specific type of abnormality in the electrical signal that regulates your heartbeat.
A delta wave is not dangerous by itself. But it can be a sign of something more serious.
What is a delta wave?
A delta wave is a type of abnormality in the electrical signal that regulates your heartbeat. This electrical signal travels through your heart and creates the normal “lub-dub” sound you hear when you place a stethoscope on your chest. The heart’s natural rhythm is called sinus bradycardia and it’s regulated by an area in the lower part of your heart called the sinoatrial (SA) node. This node controls how fast your heart beats, which is measured in beats per minute (bpm).
When this electrical signal gets disrupted, it can cause an irregular heartbeat or arrhythmia, which means there are no regular beats at all — just extra sounds (waves) on top of each other. If you’re having an arrhythmia, there may be extra sounds on top of each other during each beat (a “lub-dub” sound), or there may only be extra sounds during certain beats within each cycle (a
What does a delta wave mean on ECG?
A delta wave is a type of abnormal rhythm seen on an electrocardiogram (ECG) that occurs in the atria. The name refers to its flat, triangular shape, which looks like the Greek letter delta (Δ).
Deltas are most commonly seen in patients with atrial fibrillation (AF). They may also be seen in other heart conditions such as sick sinus syndrome, although this is less common.
What disorder produces a delta wave?
Delta waves, which are the slowest type of brain wave, are mainly associated with deep sleep. They are also produced during intense meditation and even deep hypnosis.
Delta waves are extremely slow — about one to three cycles per second. The frequency of delta waves does not vary much from person to person but can be affected by the time of day. Delta waves occur more often during sleep, especially during non-REM sleep (deep sleep).
Delta wave activity is often seen in patients suffering from schizophrenia, epilepsy, and Alzheimer’s disease, as well as other mood disorders such as depression and anxiety
Delta waves are produced by a disorder called sleep apnea. In this disorder, the airway collapses during sleep, causing a person to wake up briefly with shallow breathing. This cycle can occur hundreds of times a night, waking the person so much that they do not get enough restful sleep overall. A person who has sleep apnea may also experience insomnia and fatigue during the day due to lack of sleep.
In addition to being associated with sleep apnea, delta waves are also seen in people with epilepsy, brain injuries and certain psychiatric disorders such as schizophrenia.
Delta waves are very slow brain waves that have a frequency of 0.5 to 4 Hz. They are seen in deep sleep or coma and are not considered a normal part of the waking state.
Delta waves are found in the hippocampus, a structure in the brain associated with memory. The large amount of delta activity seen during sleep is thought to help form new memories.
How do you detect Wolff Parkinson White Syndrome on ECG?
Wolff-Parkinson-White syndrome is a congenital heart disease in which there is an abnormal connection between the upper and lower chambers of the heart. This can result in abnormal electrical signals being generated, which may result in arrhythmias (irregular heart rhythms).
The best way to detect Wolff Parkinson White Syndrome on ECG is to look for abnormalities in the ECG waves.
In Wolff Parkinson White Syndrome, there are 2 different types of waveforms that can be seen on the ECG:
P-wave – The P-wave is a small wave that represents atrial depolarization (the first part of the cardiac cycle). Normal P-waves tend to be narrow and upright in shape. In Wolff Parkinson White Syndrome, the P-wave will appear larger than normal, and may also have a slurred upstroke or downstroke.
QRS complex – The QRS complex is made up of 3 separate waves; R wave (atrial depolarization), S wave (ventricular depolarization) and T wave (ventricular repolarization). In Wolff Parkinson White Syndrome, these 3 waves may appear abnormal. For example:
R wave – If the R wave looks unusually tall (>40mm) then this
Wolff-Parkinson-White syndrome is a condition that occurs when there is an extra electrical pathway between the upper and lower chambers of the heart. This can cause irregular and rapid heartbeats (arrhythmias) that can lead to sudden death.
The extra pathway is called a pre-excitation or accessory pathway. It’s caused by a short circuit in your heart’s electrical system.
An ECG (electrocardiograph) is used to detect Wolff-Parkinson-White syndrome, but only in some cases.
What causes delta wave WPW?
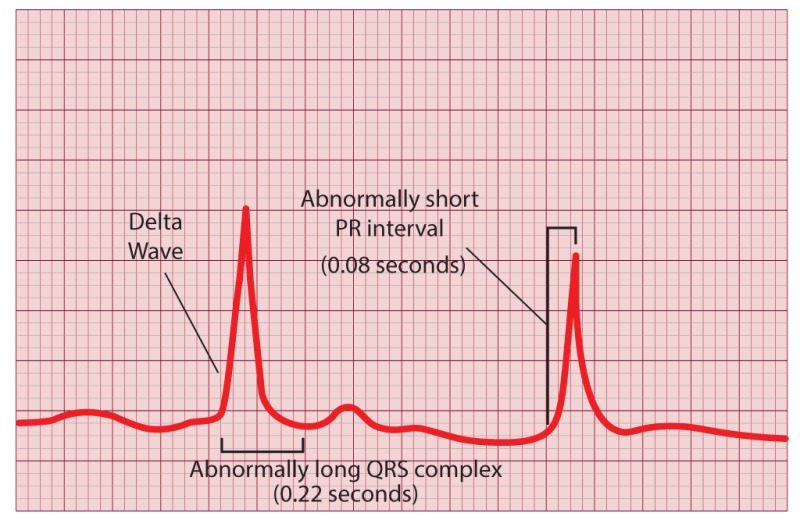
Delta wave WPW is a type of arrhythmia that can occur when an accessory pathway connects the atria and ventricles. These accessory pathways are more common in young people, but they can also occur in older people.
The electrical impulses travel across the accessory pathway instead of traveling through the AV node on their way to the ventricles. This causes an abnormal heartbeat called a delta wave.
In most cases, it isn’t necessary to treat delta wave WPW because it doesn’t cause serious symptoms or complications. Treatment can be done if you have palpitations or other symptoms from this type of arrhythmia.
What Causes Delta Wave WPW?
The main cause of delta wave WPW is an abnormal connection between the atria and ventricles (atrial-ventricular connection). This connection is called an accessory pathway or bypass tract and is made up of tissue that normally isn’t needed for normal heart function. The accessory pathway may be located anywhere along its path through the heart, including within the AV node itself (AV nodal bypass tract) or between the AV node and bundle of His (inter-atrial bypass tract). In some cases, several small accessory pathways are present but only one is functional at any given timeThe most common symptoms are palpitations — feeling like your heart is racing or skipping a beat. These can be strong and painful enough to interfere with daily activities, and they can lead to other problems like fatigue or dizziness. Delta wave WPW may also cause episodes of lightheadedness or fainting as well as atrial flutter (a fast heartbeat).
Is WPW life threatening?
WPW is not life threatening. The big concern is that if you have a ventricular fibrillation, which is the most common arrhythmia with WPW, it’s difficult to get out of it. They don’t really know what to do in that situation because there are no guidelines for it. So the main concern is that you don’t want to get into a situation where you could have a life-threatening arrhythmia and not be able to get out of it. But as long as you’re aware of your condition and you’re careful about what medications you take, then it’s not something that’s going to kill you or ruin your life.
In fact, it can be really beneficial because now we know how to treat these patients and how not to treat these patients. So now we can give them medications that don’t have side effects and that will actually help them live longer lives than they would otherwise have lived because they weren’t aware of their condition until later on in life when they needed anti-arrhythmic drugs like beta blockers or calcium channel blockersThe most common complications of WPW are abnormal heart rhythms (arrhythmias) and abnormal heart beats (cardiac arrest). Abnormal heart rhythms in WPW can be mild or severe. They may go away on their own or require treatment with medicine or an electrical shock (defibrillation). In rare cases, the abnormal heart rhythm may be life-threatening and require emergency medical care to restore normal heart function (cardiopulmonary resuscitation).
Can WPW cause sudden death?
The short answer is no.
The long answer is that it is possible for WPW to cause sudden death. However, this is very rare and only occurs under certain circumstances.
Sudden cardiac death can occur in people with WPW when there are two or more of the following conditions:
1) An abnormal heart rhythm (arrhythmia) develops that requires treatment with a pacemaker. The most common type of arrhythmia in WPW is atrial fibrillation (AF), an abnormal heart rhythm in which the upper chambers of the heart (the atria) beat too quickly and irregularly. When AF occurs, it can lead to blood clots forming in the heart and causing a stroke if they travel to the brain. If AF is not treated, it can lead to serious complications such as congestive heart failure and even death.
2) A person suffers from other medical conditions that increase their risk of developing AF such as coronary artery disease, sleep apnea or diabetes mellitus (commonly referred to as diabetes). These conditions increase blood pressure which can make it difficult for blood to flow through narrowed arteries which increases the risk of developing AF. They also increase your chances of developing atrial arrhythmias because cardiac muscle cells become weakThe risk of sudden death associated with WPW syndrome is higher in young adults (between ages 20 and 40) than in older people. This is because the condition tends to get worse with age and the risk increases as the heart becomes more damaged.
Does WPW always have a delta wave?

The delta wave is a specific type of pattern that appears on an electrocardiogram (ECG) when there are preexcited heart rhythms. It is also known as the “delta sign.”
The delta wave is most often seen with WPW syndrome. This condition occurs when there is an abnormality in the electrical pathways between the atria and ventricles. This can cause a heart rate that speeds up or slows down spontaneously, or it can cause the heart to beat too fast or too slow.
The main symptoms of WPW syndrome are dizziness and fainting. These symptoms usually occur when you stand up quickly, go from lying down to standing up (orthostatic hypotension), or exercise vigorously after resting for a long period of time (catecholaminergic polymorphic ventricular tachycardia).
People who have WPW syndrome may also experience palpitations, shortness of breath, chest pain, and chest tightness.
A delta wave is a waveform that has a slow upstroke (the steepest part of the wave) and a fast downstroke. The waves in WPW syndrome are due to an accessory pathway connecting the AV node to the ventricles, bypassing the AV junction. These accessory pathways may have different conduction properties and can result in varying degrees of heart block, depending on their location and conduction velocity.
The pattern of QRS complexes depends on where the accessory pathway is located. If it’s located above the AV junction, it can cause sinus bradycardia or complete heart block; if it’s below the AV junction, it can cause tachycardia or ventricular fibrillation.
Are delta waves present in all leads in WPW?
It is clear that a delta wave is present in all leads in WPW. It is also clear that there is no evidence for any other arrhythmia. However, it is not possible to be sure of the diagnosis of WPW from this ECG because there are no criteria that can be used to make a definite diagnosis.
The presence of delta waves alone cannot exclude the diagnosis of WPW because they are also present in other conditions such as acute myocardial infarction and hyperkalaemia. In addition, there may be other causes of right bundle branch block (RBBB) – such as left ventricular hypertrophy – with similar ECG features but which are not associated with an accessory pathway.
Delta waves are present in all leads in WPW.
Delta waves are 1-2 Hz waves. They consist of a hyperventilation phase and a diastolic phase. The hyperventilation phase is associated with the onset of atrial depolarization, while the diastolic phase is associated with atrial repolarization and the ventricular action potential.
In WPW, delta waves can be seen on all leads, but they are most prominent on V1, V3 and V4.
It is possible that delta waves are present in all leads. Delta waves are usually seen on the ECG in lead II (the lead with the highest amplitude). If you were to look at lead V1, which is located at the bottom of the heart, you may not see any delta waves.
The presence of delta waveforms is not specific for WPW syndrome. There are other conditions that can cause delta waveforms:
Heart block;
Ventricular tachycardia; and
Atrial fibrillation.
Delta waves are present in all leads in WPW.
In the normal ECG, delta waves are present only in V1 and V2 (and sometimes V3) because the left anterior fascicle is dominant in these leads. In WPW, the delta wave is also present in other leads because of the right bundle branch block morphology.
Where does WPW originate from in the heart?
WPW originates from a type of heart muscle cell called the bundle of Kent. The bundle of Kent is a group of cells in the upper right atrium that are responsible for controlling the electrical impulses that regulate heart beats.
The bundle of Kent is made up of specialised cells called Purkinje fibres. These cells form a network that transmits electrical activity from the top to bottom of the heart through the AV node and throughout the ventricles (lower chambers) of your heart.
The AV node is a small area within your heart where blood passes from one chamber to another. This node slows down and coordinates the electrical activity before it passes into each ventricle, so that both sides contract together in time with each beat.
The bundle of Kent is sometimes referred to as an accessory pathway because it can send an electrical signal directly from one side of a chamber to another through an abnormal connection known as an accessory pathway, rather than through normal connections such as those within the AV node.
WPW is caused by an accessory pathway (AP) that bypasses the AV node. This AP, called the ‘bundle of Kent,’ begins at the top of the right ventricle and extends to the bottom of the left ventricle. It also has branches to both sides of the interventricular septum.
The WPW syndrome is usually inherited genetically, but it can also develop in patients with no family history of arrhythmia.
Inherited WPW syndrome is present in 1-2% of patients who have a family history of sudden cardiac death related to syncope or SCD.
Can stress trigger WPW?

Can stress trigger WPW?
The short answer is yes. Stress can increase your risk of developing Wolff-Parkinson-White syndrome (WPW) in two ways:
- It can cause sudden cardiac arrest. If you’re running a race and get a heart attack, you may die before you have time to reach the finish line. This is called sudden cardiac arrest, and it’s caused by an arrhythmia — an abnormal heart rhythm.
The same thing can happen if you’re having a stressful day at work or school and then suddenly collapse from an abnormal heart rhythm while walking down the hall. The stress of your situation can trigger the arrhythmia that leads to cardiac arrest.
- Stress can make WPW worse over time. Some people have trouble with their hearts when they’re under stress because they have WPW syndrome. With this condition, one of the electrical pathways in your heart doesn’t work properly because of an extra pathway between your atria (top chambers) and ventricles (bottom chambers). This extra pathway makes it easier for your heart to go into a dangerous rhythm called ventricular tachycardia (VT).
