A marginal ulcer is a small sore that develops on the gum line. It may be painful and bleed easily.
The cause of marginal ulcers is often plaque buildup on the gums. Plaque is made up of bacteria and other food particles that form a hard deposit on your teeth. If you don’t brush and floss regularly, these deposits build up and can lead to gum disease.
If you have tooth decay, your dentist will likely prescribe antibiotics or an antiseptic mouth rinse to treat the infection that’s causing the ulcer. If you do not have any signs of decay or infection, there are a few things you can try at home to get rid of the ulcer:
Brush your teeth twice daily with fluoride toothpaste and floss once daily to remove plaque from between teeth and under the gum line.
Use an antibacterial mouth rinse such as Listerine or Corsodyl every day after brushing and flossing.
The treatment of a marginal ulcer is similar to that of other types of ulcers.
The most important factor in healing is keeping the area around the ulcer clean and dry. Your doctor will advise you on how to do this.
Your doctor may prescribe antibiotics if you have an infection or inflammation in your stomach lining. The antibiotic can help clear up infection and healing will occur more quickly. If you have had an operation to remove part of your stomach (gastrectomy), the wound may be open or closed with stitches or staples. In either case, it must be kept clean and dry until it heals. This usually takes several weeks but can take longer if the wound is slow to heal because of poor circulation to the area or because of infection in the wound itself.
You should not eat hot food or drink hot drinks until your bowel movements return to normal and you start passing gas normally again (flatulence). The reason for this is simple: food or drink that is too hot can cause burns inside your mouth or esophagus (swallowing tube) which might make it harder for you to heal from your ulcer
Marginal ulcers are usually caused by poor oral hygiene. They’re a common problem among elderly people who have difficulty brushing and flossing their teeth.
A marginal ulcer is an open sore that occurs at the gum line. If you have one, your dentist may prescribe antibiotic mouthwash or medication to help treat it. Your dentist may also recommend that you visit the dentist more frequently for checkups and cleanings.
The best treatment for a marginal ulcer is prevention. Brush and floss your teeth regularly, and make sure you see the dentist every six months for a cleaning.
How is marginal ulcer diagnosed?
Marginal ulcer is usually diagnosed based on a patient’s medical history, a physical examination and tests that can confirm the diagnosis.
The diagnosis may be confirmed with a biopsy. A biopsy involves taking a sample of tissue from the affected area. The tissue sample is then examined in a lab for signs of marginal ulcer.
For example, if you have an open sore on your lip, which is sometimes called angular cheilitis, the doctor may take a sample from the inside of your mouth to confirm the diagnosis.
Aside from confirming the diagnosis, biopsies can help determine whether other conditions are responsible for similar symptoms. For example, an examination of skin biopsy samples may reveal that another condition — such as eczema or psoriasis — is responsible for some of your symptoms.
Marginal ulcers are usually diagnosed by a dermatologist after a physical examination.
A skin biopsy may be taken to determine the cause of the ulcer. The biopsy will show if the ulcer is infected or has another cause, such as psoriasis or other skin diseases.
In some cases, only one test is needed to diagnose marginal ulcers:
A blood test can be done to find out if you have an infection in your bloodstream that could be causing your ulcer.
If you have a weak immune system, such as AIDS, you may have other symptoms besides the rash and sore mouth. Your doctor might also look at your blood count, which measures how many white blood cells (which fight off infections) are in your body.
Marginal ulcer is a type of skin lesion that is seen around the lips or mouth. It is often caused by an infection with herpes simplex virus (HSV).
The virus can be transmitted through kissing or sharing eating utensils.
Symptoms include:
Swollen and red lips and mouth sores that are painful and itchy.
In some cases, there may be no symptoms at all.
Treatment for marginal ulcer is usually with antiviral medication such as acyclovir which can help to speed up recovery time from the infection that causes marginal ulcers
Marginal ulcers are usually diagnosed by a physical examination of the mouth. The dentist will look for redness and irritation along the edges of the gums, as well as any open sores or wounds. The dentist may also take a small sample from the gum tissue with a scalpel or wooden stick. This sample can then be examined under a microscope to determine if it is an infection or not.
Treatment for marginal ulcers varies depending on what is causing the condition. If it is due to an infection, then antibiotics may be prescribed by your dentist. If it is due to poor dental hygiene, then regular toothbrushings and flossing will usually help heal the ulcer within several days to weeks depending on how severe it is.
Where do marginal ulcers occur?
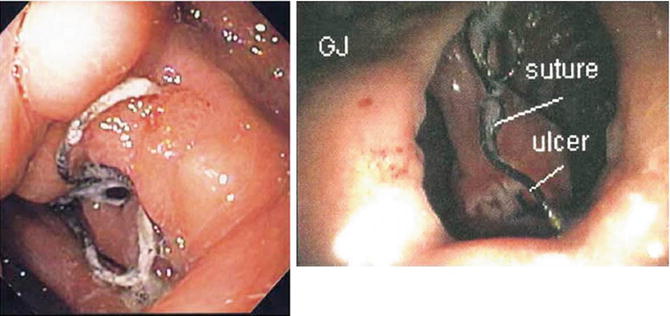
Marginal ulcers are a common form of gastric ulcer, which occur at the edge of the stomach. They develop from chronic inflammation caused by H pylori and NSAIDs.
The most common site for marginal ulcers is just below the pylorus (the part of the stomach that connects to the duodenum), but they can also occur in other places around the fundus (top) of your stomach.
Marginal ulcers are much less common than gastric ulcers.
Marginal ulcers occur in the areas of the gum where it meets the tooth. They can also develop on the gums near the cheek, tongue or other hard structures in the mouth.
If you have a history of gum disease, your risk of developing a marginal ulcer is greater. Gum disease is an infection of the gums and supporting structures that hold teeth in place. It can cause bleeding and pain, as well as loosen your teeth and eventually lead to tooth loss if not treated.
Signs and symptoms
Marginal ulcers usually start out with a small red, raised spot on your gumline that slowly becomes larger. The area around it may feel sensitive when you chew food or brush your teeth — especially if it’s located near a back molar, which helps you chew food. As it gets larger, any tissue surrounding it may become infected as well. This can lead to swelling in your cheek or neck area (where nerves are close to the surface).
Marginal ulcers are common in people with diabetes. Marginal ulcers occur at the base of the nail (the proximal nail fold) and can be difficult to see. They are caused by repeated trauma (such as banging your fingernails on the table) and result in a crack that gets infected.
Marginal ulcer symptoms include:
Painful, red, swollen base of the nail
Discharge from an infected marginal ulcer is yellow or greenish and can be foul-smelling.
Marginal ulcers are located on the margin of the oral cavity, i.e., on the lips and/or around the mouth.
They are also called angular cheilitis, which is derived from Latin words for “angular” and “cheilosis.” Angular cheilitis usually refers to a form of marginal ulceration that occurs at the corners of the mouth (angles). It can also mean any type of marginal ulceration that occurs around the mouth.
Patients with angular cheilitis often complain of pain and discomfort in their lower lip area, as well as cracking, peeling and burning sensations around their mouth. They may also notice an unusual taste or odor coming from their mouth when they eat certain foods or drink liquids other than water.
In some cases, patients may experience bleeding from their lips if they accidentally bite into them. This can lead to further inflammation and pain in addition to eating difficulties due to dryness in their mouths
Why do bariatric patients get ulcers?
Why do bariatric patients get ulcers?
Bariatric surgery is a very effective treatment for people with severe obesity. However, despite improvements in surgical techniques and better postoperative care, the risk of infection and ulceration following bariatric surgery remains high. The incidence of serious complications such as ulcers and wound infections is around 15% after gastric bypass operations and up to 30% after gastric banding.1-3 The risk of developing an ulcer after bariatric surgery is related to both the type of operation performed and the amount of weight lost. For example, gastric bypass operations result in a greater risk of developing an ulcer than banding operations because they involve more extensive surgery and weight loss.1
Why do some patients develop postoperative ulcers?
Most postoperative ulcers are caused by bacteria called Helicobacter pylori (H. pylori). H. pylori is present in the stomachs of most people worldwide but usually causes no symptoms unless people have other conditions that affect their immune system such as diabetes or iron deficiency anaemia (when there are not enough red blood cells).4 These conditions can increase the risk that small amounts of food may pass into the
Bariatric patients are at risk for developing ulcers, which is a condition that affects the lining of your stomach. The reason for this can be due to many factors.
The first thing to consider is that bariatric surgery is not a weight loss procedure, even though it is often marketed as such. Bariatric surgery reduces the size of your stomach and changes the way it functions. This means that you must change how you eat in order to ensure that you get the nutrients and calories that you need.
Here are some ways in which bariatric surgery can lead to ulcers:
1) You may not be eating enough food at one time because of the limitations placed on your stomach size.
2) Your body may not be able to absorb all of the nutrients from your food because of changes in your digestive system.
3) You may be eating too quickly or chewing too little, which can irritate your stomach lining and lead to ulcers forming.
Bariatric surgery is a last resort for weight loss. It’s reserved for people who have tried and failed to lose weight through diet or exercise, and it can be life-saving.
But despite its success in helping people lose weight, bariatric surgery is not without risks. One of the most common complications is an ulcer.
People who get ulcers after bariatric surgery are often surprised to learn that it’s a complication of the procedure itself, not something they caused on their own. But it happens to about one in five patients who have had bariatric surgery.
Here’s why you might develop an ulcer after having bariatric surgery:
Ulcers are very common in people who have had gastric bypass surgery. They can also occur in patients who have had gastric banding or vertical banded gastroplasty (VBG). The main reason for ulcer formation is because of the rapid change in the patient’s stomach size after surgery. This results in increased pressure on the stomach wall, which can lead to ulcers.
Some patients may be more prone to developing ulcers than others, but there are a number of things that can be done to help prevent them:
- Avoid smoking and chewing tobacco
- Don’t drink alcohol
- Exercise regularly
- Eat smaller meals more often
- Don’t eat foods that irritate your stomach
What does a marginal ulcer feel like?

A marginal ulcer is a shallow, irregular, painful ulcer that occurs on the side of the tongue or on the floor of the mouth.
The pain from a marginal ulcer can be mild or severe and may occur at any time during the day or night. It is often made worse by eating or drinking hot, spicy food. Some people find that their pain improves by chewing gum.
A marginal ulcer does not blanch (become white) when pressed with a tongue depressor (a wooden stick used to examine parts of the mouth).
A marginal ulcer is a red, painful area near the edge of the gum. It can be small or large and may be single or multiple.
The tissue around the edge of the gums is called the marginal gingiva. It’s sometimes called the “soft tissue” because it’s not bone. The soft tissue is made up of blood vessels, lymph vessels and nerves. The soft tissue also helps hold back plaque from getting into your teeth and underneath your gums.
When plaque builds up on your teeth, it can cause irritation in the soft tissue near your teeth and lead to inflammation. This inflammation causes pain and redness on the gum line (marginal gingiva), which may look like a red, swollen bump that bleeds easily when touched or scraped by a toothbrush or floss.
A marginal ulcer is an open sore, or ulcer, that is located on the edge of the tongue. It can also be called a “fissured tongue.”
Marginal ulcers are usually caused by poor oral hygiene. They can also be caused by certain medical conditions, such as oral cancer or diabetes.
A marginal ulcer can sometimes be mistaken for a small white spot, however, there are some key differences between these two conditions. A marginal ulcer will have a rough, crumbly surface and may bleed easily when touched. A white spot will have a smooth surface that does not bleed when touched
A marginal ulcer can be described as a sore, red area of skin that looks like a cold sore, but is smaller. It may be painful or itchy, and is usually found on the edges of the lips.
Marginal ulcers are usually caused by an allergic reaction to something that touches your lips. This can include lipstick, lip balm, toothpaste, eating spicy foods or even drinking hot drinks. They don’t usually cause any serious problems if they’re treated properly and quickly.
What causes marginal ulcers?
Marginal ulcers are caused by a reaction to something you’ve eaten or touched. They’re not caused by any sort of infection or disease, so antibiotics won’t help with them at all.
The most common cause is an allergy to something you’ve eaten or touched recently, such as toothpaste or lipstick. Eating spicy foods can also cause them in some people because capsaicin — the chemical that gives chillies their fiery kick — irritates the lips and mouth too much for some people’s liking.
What causes marginal ulcer after gastric bypass?

The most common cause of marginal ulcer after gastric bypass is poor nutritional status. This can be caused by inadequate dietary intake and/or malabsorption of nutrients.
Another common cause is infection with Helicobacter pylori, a bacteria that can infect the stomach. The bacteria can lead to inflammation and ulceration at the margins of the stomach.
In some cases, anemia can be responsible for marginal ulcer after gastric bypass. Anemia occurs when there are too few red blood cells in your body to carry oxygen to your organs and tissues. Red blood cells are produced in the bone marrow, an organ inside the bones of the body. If your body does not have enough iron or other substances needed for red blood cell production, you will develop anemia. Anemia may be caused by problems such as vitamin B12 deficiency or iron deficiency anemia (IDA).
Gastric bypass surgery (also known as gastric sleeve) is a procedure that helps people with obesity or type 2 diabetes lose weight by reducing the size of your stomach. The procedure involves stapling the stomach to create a small pouch at the top of it, which limits how much food you can eat.
The most common complication after gastric bypass is marginal ulcer, an open sore on your stomach wall where it has been stapled during surgery.
Marginal ulcers are more likely if you smoke or have diabetes before surgery.
Marginal ulcer symptoms include:
Pain in your abdomen
Nausea and vomiting
If marginal ulcers become infected, they can cause fever and chills. Marginal ulcer treatment includes antibiotics to prevent infection and pain medication so you can reduce discomfort while healing.
Marginal ulcer is a common problem after gastric bypass surgery. It occurs when the small intestine sticks out beyond part of the stomach, which has been surgically separated from it. This can cause irritation and ulceration along the “margins” or edges of the separated parts of the stomach.
The most common cause is an obstruction — blockage — between the stomach pouch and small intestine, called a biliary-enteric fistula (BEF). This occurs in about 20 percent of patients who have had gastric bypass surgery. A BEF can occur even if there was no previous history of gallstones or other gastrointestinal disease.
Other reasons for marginal ulcers include:
1) Infection with C difficile bacteria; this is more common in people who have had antibiotic treatment before surgery to prevent infection during their operation;
2) Infection with H pylori bacteria; this is more common in people who have had antibiotic treatment before surgery to prevent infection during their operation; and
3) Stress ulceration (most commonly caused by NSAIDs such as ibuprofen).
Marginal ulcers are the most common complication after gastric bypass surgery. Marginal ulcers occur when the stomach and small intestine are joined together, which can lead to leaking of food or fluid into the skin. The condition can be difficult to diagnose, but it can be treated with antibiotics and changes to diet.
Gastric bypass surgery is designed to reduce the size of your stomach, which helps you feel full sooner and makes it harder to eat large amounts at one time. This type of surgery is often used for people who have severe obesity and who have not been able to lose weight through other methods. It’s also used for people who have other medical problems related to their weight, such as diabetes or sleep apnea.
But even though gastric bypass reduces the amount of food you can eat at one time, it doesn’t prevent you from eating too much at once — especially if you’re not taking any medications or following a strict diet plan. That’s why some patients develop marginal ulcers after this procedure: They overeat because they don’t feel full enough, and then they eat too much at once and end up leaking food into their skin (or sometimes even vomiting).
The most common type of marginal ulcer
