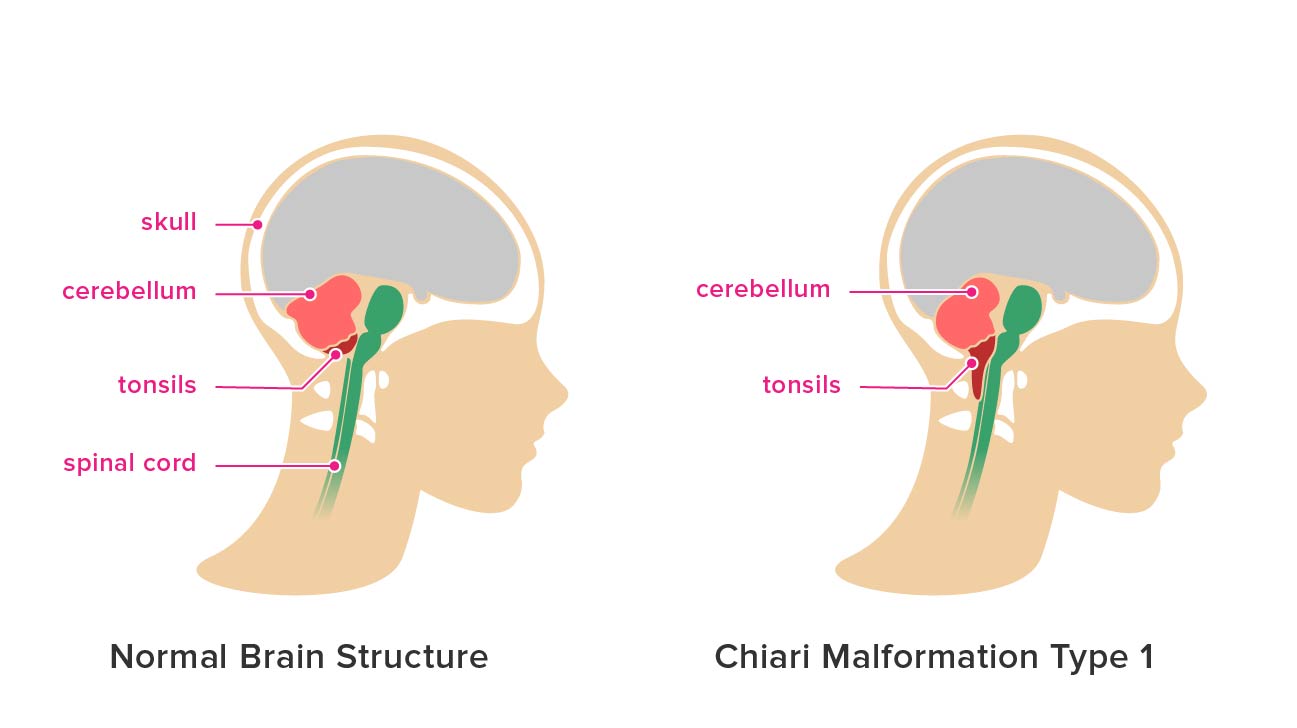
Is cerebellar tonsillar life threatening? Cerebellar tonsillar herniation is a rare form of brainstem compression. It is usually caused by a cerebellar hemorrhage, although other causes have been described as well. Cerebellar tonsillar herniation can be life threatening if not promptly recognized and treated.
Cerebellar hemorrhage can be caused by trauma, aneurysmal bleeding, or spontaneous bleeding from an unknown source. The most common cause is malignant hypertension.
Cerebellar tonsillar herniation occurs when blood within the cerebellum obstructs its passage through the foramen magnum. This results in compression of the brainstem and medulla oblongata on both sides, causing respiratory failure and potentially fatal hypoxia.
The patient may present with sudden onset of severe life headache, vomiting, ataxia and altered mental status (most commonly obtundation) due to compression of the brainstem by blood within the cerebellum. Other symptoms include hemiparesis, hemiplegia or quadriparesis depending on the degree of compression and lateralization of hemorrhage.[1][2]
The diagnosis can be made with imaging studies such as CT scan or MRI.[3][4]
The cerebellum is a part of the brain that helps control muscle movements. The tonsils are located at the back of the throat, and they help protect against viruses and bacteria that can cause illness. A cerebellar tonsil is a cerebellum that has grown into or around one of the tonsils.
Cerebellar tonsils are not common, but they can occur when there is an error in development during pregnancy. They are usually seen in children under 5 years old and rarely show up in adults.
Cerebellar tonsils may be visible on an X-ray or CT scan, but they may not be seen on a regular physical exam because they can be very small.
Most people with a cerebellar tonsil do not experience any symptoms, as they are located deep within the back of the throat where they do not get irritated by food or drink passing over them each day like normal tonsils do. In rare cases, though, people may experience pain or irritation if something rubs against their cerebellar tonsil while eating or drinking (such as if someone has an enlarged tongue).
In most cases, people with a cerebellar tonsil don’t need treatment unless it causes problems like pain or irritation while eating or
Cerebellar tonsillar ectopia is an uncommon condition with a prevalence of 0.11%. It is a congenital anomaly that causes the cerebellum to herniate through the foramen magnum. The posterior fossa of the brain is formed by the occipital bone, petrous temporal bones, and sphenoid bone. The occipital bone contributes to the superior portion of the posterior fossa, while the petrous temporal bones make up most of the inferior portion. The foramen magnum is located at the junction between these two bones. Anteriorly, it is bounded by the basilar part of occipital bone and posteriorly by anterior tubercle of atlas (C1).
The cerebellum is located in its posterior recess within the cranial cavity and rests on top of C1 vertebra (atlas). The fourth ventricle lies behind it and above it lies pons, medulla oblongata, and spinal cord (Fig 1).
What happens when necrosis happens?
Necrosis is a process of cell death that occurs in multicellular organisms. It is characterized by a blood vessel occluding and the subsequent leakage of plasma, which damages surrounding tissues. Necrosis can be caused by many different factors including trauma, infections, toxins, and autoimmune disease.
What happens when necrosis happens?
When cells undergo necrosis, they are unable to scavengel ife their internal contents quickly enough to prevent autolysis or self-digestion. This process results in the release of intracellular components such as proteins and nucleic acids into the extracellular environment. These substances can be recognized by phagocytes as foreign and lead to inflammation when they enter the bloodstream. In some cases, autophagy may occur before necrosis (wherein the cell digests its own organelles). This type of cell death is called apoptosis (programmed cell death) rather than necrosis.
Necrosis is a process of cell injury that results in the death of a portion of a tissue or organ. This process is also referred to as “tissue death”. A common result of necrosis is the formation of a cavity called an eschar, or ulcer.
In this article, we’ll look at what happens when necrosis occurs, and how it can be treated.
What is necrosis?
Necrosis is a natural process that occurs during the normal life cycle of cells. It can also be triggered by external factors such as trauma, infection or chemotherapy.
Necrosis refers to the death of all or part of a cell, often life resulting in inflammation and an inflammatory response from nearby healthy cells and tissues. Necrotic cells are known as dead at the time they are shed from living tissue or organs, although their metabolic activity may continue for some time after their appearance in the body.
Necrosis is the death of cells caused by disease or trauma. It’s usually accompanied by inflammation, which may be mild or severe. Necrosis is a process of cell death that occurs when a cell’s vital functions are irreversibly impaired. At the cellular level, necrosis is caused by a loss of homeostasis; that is, when the balance between pro-oxidants and antioxidants in a cell becomes compromised.
Necrosis can occur when tissues are deprived of oxygen life and nutrients. This condition is referred to as hypoxia (low oxygen levels) or anoxia (absence of oxygen). Tissue hypoxia may result from any condition that impairs circulation to an organ or tissue. Some examples include:
Heart attack (myocardial infarction) — A lack of blood flow due to coronary artery blockage causes hypoxic damage to heart muscle tissue, resulting in necrosis.
Stroke — Brain tissue dies because it lacks oxygen after a clot blocks an artery feeding blood to it.
Respiratory failure — This condition occurs when your lungs fail to exchange carbon dioxide for oxygen because you’re not breathing properly or because their function has been impaired by some
When cells die, they release their contents into the body. This can cause inflammation in the surrounding tissue.
Necrosis is a type of cell death that occurs when cells are damaged or die due to injury or disease.
When a cell dies, it loses its ability to control what happens life inside it. The cell membrane breaks down and releases its contents into the body.
This can cause inflammation in the surrounding tissue, which may lead to swelling, pain, redness and heat (inflammation).
What are the 4 types of necrosis?

Necrosis is the death of cells in a living tissue. It is caused by trauma, infection, toxins, cell disruption and hypoxia. Necrosis can result from a variety of conditions, including the death of some or all of the cells in a body part, as in severe burns or frostbite; some forms of heart attack and stroke; diffuse damage to neurons in the brain following oxygen deprivation (as in carbon monoxide poisoning); multiple organ failure; or systemic inflammatory response syndrome (SIRS).
There are four types of necrosis: coagulative necrosis (or dry), caseous necrosis (or cheesy), liquefactive necrosis (or slushy) and autolytic necrosis (or self-digestion).
Necrosis is a form of cell injury which results in the premature death of cells in living tissue by autolysis. Necrosis can be caused by infection, toxins and other factors that result in a disruption to the normal process of cell metabolism.
There are four types of necrosis:
Fibrinolytic (inflammatory) necrosis – This type of necrosis occurs when there is an overproduction of fibrin within the tissues. This can be caused by trauma or infection.
Apoptotic or programmed cell death – Apoptosis is a highly regulated series of events that results in the elimination or “death” of cells. It occurs as part of normal development life and growth as well as from external influences such as infection, toxins and radiation.
Coagulative (clotting) necrosis – This type of necrosis occurs when life there is an interruption in blood flow through a tissue due to thrombosis (a blood clot), embolism (particulate matter) or vasoconstriction (constriction of blood vessels). The affected area becomes damaged due life to hypoxia (lack of oxygen) and eventually undergoes liquefaction (dissolution).
Necrosis is the death of tissues due to a lack of oxygen, generally life due to an interruption in the blood supply. The three main types of necrosis are acute, subacute, and chronic.
Acute necrosis occurs suddenly and is usually caused by physical trauma or infection. It results in rapid cell death, but since the body’s normal healing processes aren’t activated, it can lead to scarring and deformity. Acute necrosis can also be caused by heat damage or exposure to toxins such as alcohol or drugs
Subacute necrosis occurs over a period of days or weeks and is typically caused by long-term stress on tissue, such as from pressure on a bone or tendon
Chronic (indolent) necrosis is slow-growing and may not cause any pain until it affects an important organ like the liver or kidney
What happens during necrosis?
Necrosis is a type of cell injury that results in the premature death of cells. Necrosis life can be caused by external or internal factors, such as infection and toxins.
External factors include:
Trauma. Damage to tissues and organs can result in life necrosis, especially if it’s severe enough to disrupt blood flow or oxygen supply to an area. Trauma-related necrosis is often referred to as coagulative necrosis. Coagulative means that the tissue becomes clotted with fibrin (a protein that helps stop bleeding) or other blood products that block oxygen flow in the area.
Physical damage to cells is one example of how physical trauma can lead to cell death. For example, if you sprain your ankle, your foot may swell rapidly from increased fluid pressure within your leg’s veins and arteries. This swelling damages nearby tissues and compromises their ability to receive oxygenated blood from your heart. Without oxygen, cells begin dying off rapidly — a process called coagulative necrosis — which may result in severe pain and swelling for days or weeks after the initial injury occurred.
Exposure to high temperatures also causes life necrosis by damaging proteins within cells so much that they lose their ability to function properly. This type of cell damage is called thermal
Necrosis is the death of a cell or tissue. Unlike life apoptosis, necrosis is an unprogrammed response to cellular injury that causes premature cell death. Necrosis can be caused by physical trauma, infection, toxins and other stressors. Necrotic cells swell as they die and release their contents into the surrounding area, causing inflammation that can damage surrounding tissues.
Necrosis can occur in any type of tissue, including muscle, bone and cartilage. Examples include:
Cell death caused by physical trauma (examples: crush injuries)
Cell death caused by inflammation (examples: burns, frostbite)
Cell death caused by infection (examples: gangrene)
Necrosis is a form of cell injury that results in the premature death of a cell, generally due to external factors. Necrosis is often characterized by swelling and redness at the site of the cell death.
Necrosis and apoptosis life are types of programmed cell death (PCD), which occurs when cells deliberately kill themselves. Apoptosis is usually triggered by internal signals, while necrosis is usually caused by external stimuli such as trauma or toxins.
Necrosis vs apoptosis
Necrosis has several distinguishing characteristics that distinguish it from apoptosis. The first difference between these two types of cell death is the time frame during which they occur. Necrosis life can occur immediately after an injury, while apoptosis may take hours or even days. A second difference is that necrosis occurs only when the cell membrane is disrupted, while apoptosis can happen without any physical damage to the membrane.
A third difference between necrosis and apoptosis is that necrotic life cells do not release proteins into their immediate environment like apoptotic cells do, so there are no “signals” sent outside of the cell during necrosis. Finally, necrotic cells usually have blebbing on their surface with loss of organelles or cytoplasmic vacu
Is necrosis always fatal?
Necrosis is the death of living tissue. It can be caused by a number of conditions, including trauma, infection and autoimmune diseases.
Necrosis can also be caused by exposure to certain chemicals or radiation. In some cases, it may be an adverse reaction to a medication or an environmental toxin.
The death of cells in necrosis can lead to a range of symptoms, including pain and swelling at the site of injury, discoloration and even bleeding.
In many cases, necrosis is not life-threatening. life However, if left untreated, it can lead to other complications that are potentially fatal. If you suspect that you have necrotic tissue in your body — especially if it is painful or causing other symptoms — contact your doctor right away.
Necrosis is a type of cell injury that occurs in response to certain kinds of physical trauma. Cells can die due to necrosis when they are deprived of oxygen, which results in the release of chemicals that kill them.
There are two types of necrosis: focal and diffuse. Focal necrosis occurs when only part of a cell dies; diffuse necrosis kills all or most of the cells in an area.
Focal Necrosis
Focal or regional necrosis involves only part of the cell dying and life leaving behind what looks like a ghostly white outline. The rest of the cell may be healthy, but it cannot carry out its normal functions because there is no longer enough tissue for it to connect with other cells or tissues in order to do so. This type of necrosis can occur in any organ or tissue and may be caused by infection, trauma or cancerous growths (tumors).
Diffuse Necrosis
In diffuse necrosis, all or most of the cells in an area die and are replaced by fat tissue and scar tissue over time as new cells grow around them. This type of necrosis occurs when there is not enough oxygen (hypoxia) for needed metabolic processes to occur within cells, leading to their death
What necrosis looks like?

Necrosis is the death of cells, which causes cells to become damaged and die. Necrosis can occur in any organ or tissue.
Necrosis is not a specific disease, but rather a symptom of an underlying problem. The causes of necrosis vary widely, but they are often associated with some kind of injury or trauma. The tissue damage caused by necrosis can range from mild to severe depending on the cause and extent of the injury.
The signs and symptoms of necrosis vary depending life on what life type of cell is affected and how much damage has occurred.
Common signs and symptoms include:
Discoloration (for example, yellowing)
Pain and tenderness
Heat or swelling at the affected area
Necrosis is the death of cells or tissue. There are two types of necrosis: acute, which is characterized by inflammation, and chronic, which involves degeneration.
Acute necrosis is a common symptom of many diseases and can be fatal life if left untreated. It can occur in any organ system, but it most often affects the skin, heart and brain.
Chronic necrosis may be caused by viruses or bacteria. It can also be caused by physical injury to body tissues, such as burns or radiation damage.
Necrosis is a type of cell death that occurs when certain cells in the body die, but the body does not properly remove the dead cells. This can lead to inflammation and infection.
The following are signs and symptoms of necrosis:
Pale or yellowish skin color
Skin lesions (such as blisters, ulcers or open sores)
Itching or burning sensation
Painful skin lesions
Necrosis is the death of cells or tissue in a life localized area. Necrosis occurs when a cell is damaged and its internal contents spill out. The surrounding tissue then becomes inflamed, causing it to swell and form a blister.
If the damage is not repaired, necrosis can lead to infection, which can spread to other areas of your body.
Signs and symptoms
Necrotic skin may appear dry, grayish-brown or blackened, with an uneven surface that feels firm and leathery. The area may be swollen and painful to the touch.
Does necrosis need to be removed?
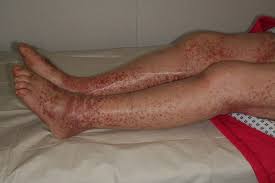
Necrosis is death of cells and tissue, usually life resulting from injury or infection. Necrosis can be categorized as acute or chronic. Acute necrosis is sudden and progressive while chronic necrosis develops slowly over time. The symptoms of necrosis are pain, inflammation, swelling, redness and heat.
Necrotic tissue may appear yellowish-brown in color and firm to touch. Necrotic tissue can have a foul smell due to the release of bacteria into the area. If life necrotic tissue is not removed, it can lead to further complications such as abscesses and infection.
It is important for patients with necrotic tissue life to receive proper care by an experienced physician who can diagnose the underlying cause of their condition life and recommend appropriate treatment options that will address their individual needs.