Have you ever heard of Mesothelioma? If not, you’re not alone. This rare form of cancer often flies under the radar, but its impact is anything but insignificant. It’s a silent predator, often lying dormant for decades before rearing its ugly head. And when it does, it’s a surprise explosion that leaves patients and their families reeling.
But there’s hope. Mesothelioma surgery is often a lifeline thrown to those grappling with this disease. This article will delve into the complex world of mesothelioma surgery, discussing its necessity, the process involved, the risks, and the aftermath. We’ll take a deep dive into why surgery is often the chosen method of treatment, the different types of surgeries available, and what you can expect during recovery and aftercare.
So, why is surgery necessary? Well, think of mesothelioma as a bomb. It’s ticking away inside the body, causing damage and destruction. Surgery is the bomb squad, diffusing the threat and removing the danger. It’s a complex, intricate process that requires skilled surgeons and advanced medical technology. But when successful, it can make a world of difference. Are you ready to explore this fascinating topic? Let’s dive in!
Understanding Mesothelioma
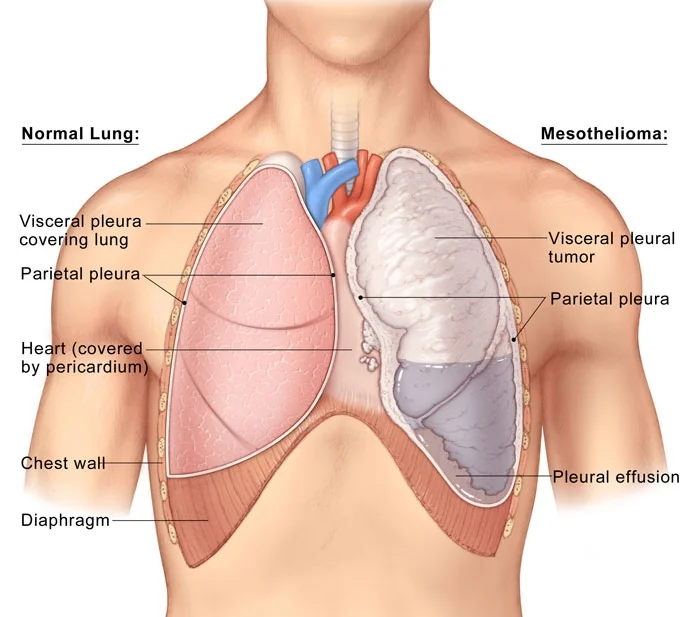
Before we delve into the intricacies of mesothelioma surgery, it’s essential to first understand what mesothelioma is and how it affects the body. Mesothelioma is a rare but aggressive form of cancer that primarily affects the lining of the lungs and abdomen, known as the mesothelium. It’s primarily caused by exposure to asbestos, a naturally occurring mineral that was widely used in construction and other industries until its dangers were fully recognized.
The disease can take decades to manifest, often making diagnosis a challenge. When asbestos fibers are inhaled or ingested, they can become lodged in the mesothelium, causing cellular damage and leading to the development of cancerous cells. The result is a rapid and uncontrolled growth of cells, leading to a buildup of fluid and the formation of tumors.
Patients with mesothelioma often experience symptoms such as chest or abdominal pain, shortness of breath, and unexplained weight loss. Unfortunately, due to the late-stage diagnosis, the prognosis for mesothelioma patients is often poor. However, treatments like surgery can help manage the disease and improve the quality of life for patients.
Why Surgery is Necessary
This section will explore the reasons why surgery is often the chosen method of treatment for mesothelioma. Mesothelioma is a serious type of cancer that primarily affects the lining of the lungs and abdomen. As with most cancers, early detection is key to a successful outcome. However, due to the slow-developing nature of mesothelioma, it often goes undiagnosed until it has progressed to advanced stages. At this point, the disease may have spread to a point where non-surgical treatments, such as chemotherapy and radiation, may not be as effective.
Surgery is therefore necessary to remove the tumor and potentially any surrounding tissue that may be affected. This method of treatment can significantly improve the patient’s quality of life and increase their chances of survival. It’s important to note that not all mesothelioma patients are suitable candidates for surgery. Factors such as the patient’s overall health, the stage and location of the cancer, and the patient’s personal wishes are all taken into consideration when deciding on the best course of treatment.
There are several types of surgeries used to treat mesothelioma, each with its own benefits and risks. These include pleurectomy, extrapleural pneumonectomy, and cytoreductive surgery with HIPEC. The choice of surgery depends on a variety of factors, including the stage of the disease, the patient’s overall health, and the surgeon’s expertise.
Types of Mesothelioma Surgeries
When it comes to treating mesothelioma, there are several surgical options available. Each comes with its own set of benefits and risks, and the choice often depends on the stage and location of the cancer, as well as the patient’s overall health. Let’s dive into the details.
The first type of surgery is Extrapleural Pneumonectomy (EPP). This is a major surgical procedure where the diseased lung, part of the pericardium, (the membrane covering the heart), part of the diaphragm (muscle between the lungs and the abdomen), and part of the parietal pleura (membrane lining the chest) are removed.
Next, we have Pleurectomy/Decortication (P/D). This surgery involves the removal of the pleura and all visible tumor masses. Unlike EPP, P/D spares the lungs. It’s considered a lung-saving surgery and is often preferred when the disease is detected early and the patient’s lung function is good.
Another type of surgery is Cytoreductive Surgery with Hyperthermic Intraperitoneal Chemotherapy (HIPEC). This is used for peritoneal mesothelioma and involves removing as much of the tumor as possible followed by a heated chemotherapy solution that is administered directly into the abdominal cavity.
Lastly, there’s Debulking. This surgery aims to remove as much of the tumor as possible to relieve symptoms and improve the patient’s quality of life. It’s often used when the disease is too advanced for curative surgery.
Remember, each surgical procedure comes with its own set of risks and potential complications. It’s important to discuss these with your doctor to make an informed decision about your treatment.
Risks and Complications
Like any surgical procedure, mesothelioma surgery carries certain risks and potential complications. We’ll discuss these in this section. It’s essential to understand that while surgeons and medical teams do their utmost to minimize risks, complications can occur. The complexity of the surgery, the patient’s overall health, and the stage of the disease can all influence the outcome.
Some of the common risks associated with mesothelioma surgery include:
- Bleeding: This is a risk with any surgery, but because mesothelioma often involves the lungs, the risk can be higher.
- Infection: Despite the best efforts of the surgical team, infections can occur post-surgery.
- Reactions to anesthesia: Some patients may have adverse reactions to the anesthesia used during the procedure.
- Respiratory complications: Given the location of the surgery, some patients may experience difficulty breathing post-surgery.
It’s crucial to discuss these risks and potential complications with your healthcare provider before deciding on surgery. It’s also important to remember that while these risks exist, surgery often provides the best chance of extending life expectancy and improving quality of life for patients with mesothelioma.
Recovery and Aftercare
Once the surgical dust has settled and the operation is but a memory, the real work begins – the recovery and aftercare. This phase is just as important, if not more so, than the surgery itself. It is during this time that the body begins to heal and adapt to the changes made during the operation.
So, what can you expect during this critical period? Well, let’s start with the basics. Immediately after the surgery, you’ll likely be groggy and tired. This is normal. Your body has just been through a major ordeal and needs time to recover. You’ll be closely monitored by the medical team to ensure everything is progressing as it should.
As you regain your strength, you’ll start to notice some changes. You may experience pain and discomfort in the area where the surgery was performed. This is also normal and can be managed with medication. You may also notice changes in your appetite and energy levels. Again, this is part of the healing process and will improve over time.
Now, let’s talk about aftercare. This is the long-term care plan that’s put in place to ensure you continue to heal and improve after you’ve been discharged from the hospital. This may involve regular check-ups with your doctor, medication, physiotherapy, and possibly even changes to your diet and lifestyle.
Remember, every person’s recovery and aftercare journey is unique. What works for one person may not work for another. The key is to listen to your body, follow your doctor’s advice, and give yourself the time you need to heal.