Revolix Laser Prostate Surgery is a minimally-invasive, outpatient procedure that uses a laser to remove the prostate gland. The procedure involves removing the entire prostate gland or a portion of it.
The Revolix Laser Prostate Surgery is performed through a small incision in the perineum (the area between the scrotum and anus). The surgeon uses a special device to make a series of precise cuts in the lining of the prostate gland, allowing him or her to remove the gland with minimal bleeding and damage to surrounding tissue.
To learn more about Revolix Laser Prostate Surgery and other treatment options, talk with your doctor today.
The Revolix laser prostate surgery uses a high-definition video camera to create a 3D image of the prostate and surrounding anatomy. The surgeon can then see the exact position of all critical structures, allowing for precise placement of instruments and implants.
The Revolix laser prostate surgery is performed in the operating room, under general anesthesia and with full sterile precautions. A small incision is made in the lower abdomen through which the laser probe is inserted. The probe has an optical head that transmits images to a computer monitor, allowing the surgeon to view real-time images while performing the procedure.
The surgeon begins by inserting a special device into the rectum (sphincterotomy) to relax the muscle so that it can be moved out of the way during surgery. During this portion of the procedure, no incisions are made; instead, instruments are inserted through tiny openings in order to remove tissue from inside the prostate. Once all necessary tissue has been removed from inside the organ, it is rebuilt by sewing together any tears or holes in its outer lining (capsule).
Revolix Laser Prostate Surgery
Prostate surgery is the most common urological procedure performed in the United States. The prostate gland is located below the bladder, and it surrounds the urethra, which is a tube that carries urine from the bladder to the penis.
The prostate gland produces about one-third of all semen (the fluid that contains sperm). The prostate also helps produce seminal fluid, which helps nourish and transport sperm.
In most cases, prostate cancer develops in men over age 50. It is the second leading cause of cancer deaths among men in the United States, behind only lung cancer. Most men who develop prostate cancer don’t have any signs or symptoms until their disease has spread beyond the prostate gland into surrounding tissue or other areas in the body (metastasized).
Prostate surgery is the most common surgical procedure performed on men in the United States. The prostate, a small gland about the size of a walnut that surrounds the urethra, produces fluid that is part of semen.
A number of options are available for treatment of prostate cancer. These include watchful waiting, active surveillance, radiation therapy and surgery. Surgery is usually performed to remove all or part of the prostate gland if cancer is diagnosed during an examination of the gland (known as a transrectal ultrasound-guided biopsy). This can be done using three different approaches: through the abdomen, through the urethra (known as transurethral resection) or through an incision made in the rectum (called robotic assisted laparoscopic radical prostatectomy or RALP).
The type of surgery depends on several factors, including:
• the size and location of your tumor and nodules
• your overall health
• whether you want to preserve sexual function
• whether you want your bladder to store urine after surgery
What is the success rate of laser prostate surgery?
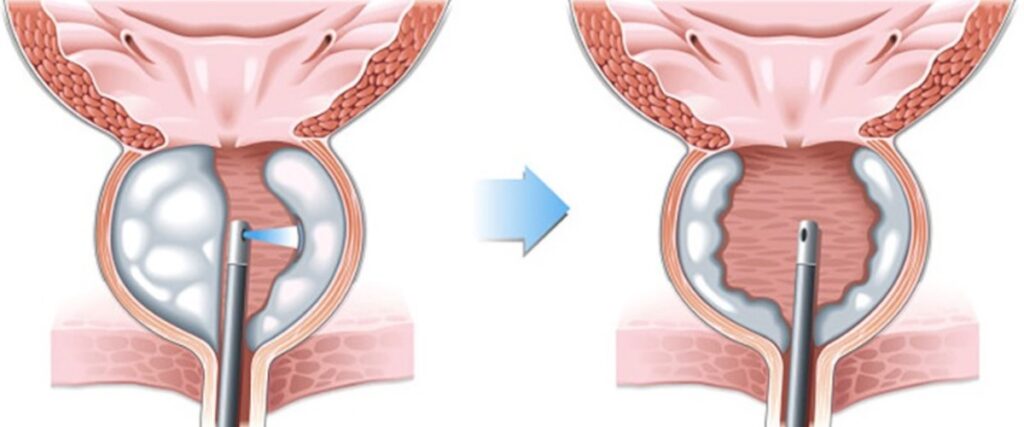
Laser prostate surgery is a relatively new procedure that is gaining popularity among physicians and their patients. The procedure uses a laser to treat cancerous tumors in the prostate by destroying them without damaging healthy tissue.
Laser prostate surgery is not for everyone, but it can be an effective treatment option for some men with early-stage prostate cancer that has not spread beyond the gland.
The success rate of this procedure depends on several factors, including the stage of cancer, whether or not it has spread to other organs and the patient’s overall health. In general, laser surgery has an 85% cure rate after five years, which is comparable with other treatments such as external beam radiation therapy (EBRT).
Below we answer some common questions about laser surgery:
What is the success rate of laser prostate surgery?
Laser prostate surgery is a minimally invasive procedure that uses a laser beam to remove cancerous tumors. It is considered a very effective treatment for early-stage prostate cancer, but it can also be used in other stages depending on your specific situation.
The success rate of laser prostate surgery depends on many factors, including your overall health and the type of cancer you have. If you have localized cancer that has not spread outside the prostate, then your chance of survival is likely to be around 100%. If there are other symptoms such as bone pain or urinary incontinence, then they may be addressed with additional treatments such as radiation therapy or hormone therapy.
If there are no symptoms present, then it may be possible to avoid further treatment altogether, especially if you have an early stage disease with low-risk features like Gleason score 6 (2 or 3). Your doctor will determine whether or not you need any further treatment after examining your medical history and biopsy results
The success rate of laser prostate surgery is high for the majority of men. This type of surgery is less invasive than surgical removal and does not involve cutting through muscle tissue. However, because it is a minimally invasive procedure, there are still risks involved.
The success rate for laser prostate surgery depends on the experience of your surgeon and whether you are a good candidate for this type of treatment. If you do not meet the criteria for laser prostate surgery, then you may be better served by traditional open surgery.
The success rate for laser prostate surgery is about 95 percent for those who are good candidates for the procedure. The most common complications are bleeding or infection around your urethra or bladder. Bleeding can occur during or after surgery and will require additional treatment to stop bleeding in these areas. Infection near your urethra or bladder can also occur if you have an open wound or an infection at another location in your body that becomes infected while you are undergoing treatment.
The success rate of laser prostate surgery is very high. According to a study published in the Journal of Endourology in 2014, the three-year failure rate for laser prostate surgery was just two percent.
The success rate for laser prostate surgery is influenced by several factors, including:
Age — Older men tend to have more problems with incontinence after laser prostate surgery than younger men do.
Disease stage — Men with less advanced disease are likely to have better results than those whose cancer has spread beyond the prostate gland.
Laser treatment — Men who receive one or more treatments to destroy cancer cells may have a lower likelihood of developing side effects such as incontinence and impotence than those who only receive one treatment.
How long does it take to recover from prostate laser surgery?
The recovery time for laser prostate surgery is typically very short. The majority of patients can return to work within a few days, and they may be able to resume sexual activity as soon as one week after the procedure.
Laser prostate surgery is not an invasive procedure, so it should be relatively easy to recover from. The main thing you need to avoid during your recovery period is any activity that might result in a strain or injury. You’ll also need to take medications that help reduce the risk of infection and other complications.
The average length of time people spend recovering from laser prostate surgery is about two weeks, but this varies depending on what type of medical treatment they received before their operation. Some men may need up to six weeks before they’re fully recovered.
Many men who choose this kind of treatment report a high degree of satisfaction with their decision, but there are some risks involved as well. If you want more information about laser prostate surgery, talk with your doctor about your options and how long it will take for you to recover from this type of procedure
Prostate laser surgery is a common treatment for prostate enlargement that can cause symptoms such as frequent urination and difficulty starting urine flow. It’s also sometimes called transurethral resection of the prostate (TURP).
Laser prostate surgery is an outpatient procedure that usually lasts about 30 minutes. The time it takes to recover depends on the type of laser used, your age and general health, and how well you follow your doctor’s instructions after surgery.
Recovery time for laser prostate surgery
Most men return to their normal activities within one to two weeks after laser surgery. However, you may need up to three months to recover from the effects of anesthesia and pain medicine after the procedure. It may take longer if you have other medical conditions or if you smoke cigarettes.
Some men are able to resume sexual activity within a few weeks after laser prostate surgery. However, if you had severe incontinence before the procedure or have leakage afterward, it may take longer for your bladder function to improve enough for sex without leaking urine during intercourse.
Prostate laser surgery (also known as prostatectomy) is a surgical procedure to remove the prostate gland. The surgeon uses a laser to make a small cut in the skin of the abdomen and then inserts a thin, flexible tube called a resectoscope into the body through this incision. The resectoscope has an attached light and camera that allows the surgeon to see inside your body.
The surgeon passes instruments through the resectoscope to cut out the cancerous prostate gland and surrounding tissue. After removing as much of the cancer as possible, he closes up your abdomen with stitches or staples.
You may have some pain or discomfort after surgery or need pain medicines for several days after surgery. Your doctor may recommend that you take stool softeners or laxatives over the next few weeks to prevent constipation while your bowels heal from surgery.
It is normal to have some pain and discomfort after surgery, but you should be able to get out of bed and go to the bathroom on your own within 24 hours. You may need to use a catheter for several days after surgery.
You should be able to resume light activity, such as walking and riding an exercise bike, within a week or two of your surgery. Your doctor will tell you when it’s safe for you to return to work and begin sexual activity.
Most patients recover fully from prostate laser surgery within a few weeks.
What is the best laser surgery for prostate?

The best laser surgery for prostate is one that removes the cancer with a minimum amount of surrounding tissue. This means that the surgeon should be experienced with this technique and should have a high cure rate.
A transurethral resection of the prostate (TURP) or open surgical removal of the prostate (RRP) are both good options for treatment of benign prostatic hyperplasia (BPH). TURP is usually performed in an outpatient setting and requires a catheter to drain urine from the bladder. RRP is an open procedure that may require hospitalization, but it has a lower risk of complications than TURP.
There are several types of lasers used in urology today, including argon and holmium lasers.
Prostate cancer is the second leading cause of cancer death among American men, after lung cancer. The American Cancer Society estimates that there will be 233,000 new cases of prostate cancer diagnosed in 2018 and that 27,540 men will die from this disease this year.
Prostate cancer is usually very slow growing and often does not need to be treated. But if it grows quickly or spreads to other parts of your body, it can become life threatening.
The most common treatment for prostate cancer is surgery to remove all or part of the prostate gland. Your doctor may recommend a transurethral resection (TUR) as an alternative to open surgery. This type of surgery uses a laser instead of traditional scalpel blades to remove tissue from your prostate gland.
Laser surgery for prostate has been around for many years but has recently become more popular because it’s less invasive than traditional TURs. In fact, some urologists believe that laser surgery for prostate offers several advantages over traditional surgery:
Less pain during recovery — Traditional TURs require cutting through tissue with a scalpel blade, which causes bleeding and pain during recovery. Laser surgeries don’t use scalpels so they don’t cause bleeding or require stitches afterward
The best laser surgery for prostate is the Holmium laser.
This is a new technique that was developed by Dr. David Samadi, M.D., F.A.C.S., a leading urologist at Lenox Hill Hospital in New York City and a member of the Fox News Medical A-Team.
The Holmium laser has been shown to be superior in every way over other procedures like transurethral resection (TUR) or TURP, which have been around for over 40 years. The Holmium laser offers patients:
Less blood loss
Less pain
Shorter recovery time
The best laser surgery for prostate is the one that is right for you.
The main three types of treatment for prostate cancer are:
Watchful waiting
Active surveillance
Surgery
Watchful Waiting
Watchful waiting is not a treatment option, but rather a way of managing your condition. Watchful waiting means that we monitor your symptoms and wait to see if they get worse or not. If they do, then we will recommend active surveillance or surgery. This can be a good option if you have a low-risk form of prostate cancer, but it does mean that you need to have regular tests to check that your cancer has not become more aggressive. You may also need further treatment if you develop any symptoms such as needing the toilet more often than usual or having difficulty passing urine. A small number of men with low-risk prostate cancer will develop symptoms which require further treatment at some point during this period. However, most men do not develop symptoms during this period and will only need treatment if their cancer progresses beyond being low risk after 5 years of being under observation (active surveillance).
Which is better TURP or laser?
TURP is a surgical procedure to remove the prostate gland. It’s done on an outpatient basis, and the patient can go home the same day.
A laser is a surgical tool that uses light energy to remove tissue. A laser can be used in either a TURP or open surgery to remove prostate tissue.
Both TURP and laser offer advantages and disadvantages. The right choice for you depends on your age, overall health and how much cancer is present in your prostate.
There are currently three types of laser treatments for prostate cancer:
Transurethral resection of the prostate (TURP) – A surgical procedure in which the surgeon makes small incisions in the urethra and bladder neck to remove the obstructing tissue from inside the prostate.
Radiofrequency ablation (RFA) – An alternative surgery that uses heat from radiofrequency energy to destroy tissue.
Laser-assisted resection of the prostate (LARP) – A minimally invasive procedure that uses a laser probe to vaporize tissue that blocks urine flow from the bladder, allowing urine to flow freely out through the urethra.
Laser surgery is a minimally invasive procedure that uses a laser beam to heat a precise area of the prostate. The laser treatment can also be performed with a robotic system known as da Vinci.
Lasers used for prostate surgery include holmium lasers, which are often used in urologic procedures, and neodymium:yttrium-aluminum-garnet (Nd:YAG) lasers.
Lasers are energy devices that emit light in the form of photons. When the photons strike your tissue, they excite its molecules and cause them to vibrate and heat up. The heat destroys the tissue and leaves behind healthy tissue with minimal scarring.
TURP stands for transurethral resection of the prostate, which is a surgical procedure to remove part or all of the prostate. The surgeon uses a cystoscope that is inserted into the urethra, which allows them to see inside your bladder and prostate gland. Then they use special tools to cut out pieces of tissue from your prostate gland that are blocking urine flow.
Laser surgery is also called photoselective vaporization of the prostate (PVP). It’s used to treat an enlarged or cancerous prostate gland. In this procedure, the doctor inserts a laser fiber through your urethra and uses it to burn away small areas of tissue in your body.
Both TURP and PVP are minimally invasive techniques that can help you avoid major surgery. You may have heard these procedures referred to as “laser surgery” or “surgery without cutting” because they don’t require an incision in your skin. Both procedures are typically done on an outpatient basis with no overnight stay at the hospital required
Can you have a normal life after prostate surgery?

It can take up to three months to recover from prostate surgery.
You should be able to return to normal activities, such as driving and going back to work, within a week or two. It may take longer if you have had a radical prostatectomy or nerve-sparing surgery because of the risk of incontinence (inability to control urination) and erectile dysfunction.
You should be able to resume sexual activity within six weeks of surgery, but it may take longer if you’ve had nerve-sparing surgery or radiation therapy.
It’s important to talk with your doctor about the type of recovery you can expect after having surgery for prostate cancer.
The prostate gland is a part of the male reproductive system. It’s about the size of a walnut and is located just below the bladder and in front of the rectum.
Prostate surgery may be needed if you have an enlarged prostate or cancerous cells in your prostate. The procedure can be done through either an open incision or laparoscopically.
The main types of prostate surgery are:
Transurethral resection of the prostate (TURP). This type of surgery uses a small surgical instrument called a resectoscope to remove tissue from inside your bladder that’s blocking urine flow. A laser may be used to seal off blood vessels or help remove extra tissue, which may cause overflow incontinence.
Open prostatectomy (also known as radical prostatectomy). An incision is made on one side of your lower belly to remove the entire gland and part of the urethra, through which urine flows out of the body. Your surgeon will close this incision with stitches or staples, but no external support such as packing material will be required after surgery because there are no large open spaces left at the end of your urethra where bacteria can grow unchecked as in women who have had vaginal
Prostate cancer is often a slow-growing disease. But it can become a serious health threat if left untreated or if it spreads outside the prostate gland.
The most common treatment for prostate cancer is surgery to remove the prostate gland. The goal of surgery is to cure the cancer by removing all of it or as much of it as possible while preserving sexual function and bladder control.
Some men opt for a radical prostatectomy, which completely removes the prostate gland and surrounding tissues. Others may choose a less invasive approach, such as robotic surgery or laparoscopic surgery with robotic assistance (RARP). RARP uses smaller incisions than traditional open surgery and has less blood loss and quicker recovery time than open surgery does.
Men with prostate cancer who have a radical prostatectomy or radiation therapy may have some temporary side effects after treatment. These include:
The immediate aftermath of surgery can be painful, and you may need pain medicine for several days. You may also need to take antibiotics to prevent infection.
Urinating may be difficult for the first week or two after surgery. You’ll probably need to empty your bladder often and use a catheter for the first few days after surgery. A male nurse will teach you how to use the catheter, which is inserted into your urethra (the tube that carries urine out of your body). It’s important that you do not try to push urine through the catheters by squeezing them with your hands or fingers — this could cause serious damage!
Infection is always a risk after surgery, so you’ll need to take antibiotics as directed until they’re finished. Your doctor will probably order a test called a PSA (prostate-specific antigen) blood test before you leave the hospital and periodically afterward to monitor changes in your PSA level — this test measures levels of an antigen produced by normal cells as well as cancerous prostate cells.
What is the newest surgery for enlarged prostate?
Prostate surgery is one of the most common procedures performed in the United States. The purpose of the procedure is to remove all or part of the prostate gland and may be done for various reasons.
The most common reason for performing a total prostatectomy is cancer, but non-cancerous conditions such as benign prostatic hyperplasia (BPH) are also treated with this surgery.
The type of surgical procedure used for removing the prostate depends on several factors, including:
Size and location of the tumor
Symptoms present before surgery
Age of patient
What is the newest surgery for enlarged prostate?
The newest surgery for enlarged prostate is called a “minimally invasive robotic prostatectomy.” The surgeon makes an incision in the lower abdomen, and a special camera on a robotic arm is placed inside the body. The surgeon then operates on the prostate through this incision. It is similar to traditional laparoscopic surgery but with much less discomfort and recovery time.
This type of surgery has been shown to have fewer complications than traditional open surgery, including fewer urinary tract infections and less blood loss. The procedure also often causes less pain afterward because there is no need for large incisions in the abdomen.
The newest surgery for enlarged prostate is transurethral microwave thermotherapy (TUMT). It’s called a “mild” treatment because there’s no incision and it’s less invasive than other treatments.
The TUMT procedure is performed by inserting a hollow tube into the penis that has a probe at the end. The probe delivers high-frequency energy to the prostate tissue, causing it to shrink. The surgeon then removes any excess tissue through the same incision he used to insert the probe into your urethra.
The entire procedure takes about 10 minutes and is usually done on an outpatient basis with local anesthesia as opposed to general anesthesia, which means you’ll be awake but relaxed during the surgery and won’t remember much about it afterward.
TUMT has been shown in studies to be very effective at treating lower urinary tract symptoms caused by benign prostatic hyperplasia (BPH), including frequent trips to urinate, difficulty starting urination, feeling like your bladder isn’t empty after going to the bathroom, having trouble emptying your bladder completely and having problems in bed such as waking up several times during the night to urinate or waking up with a full bladder that doesn’t go away after drinking large amounts of fluids before going
There are two main types of surgery for enlarged prostate. One is transurethral resection of the prostate (TURP), which involves removing part of the prostate through a tube inserted into the urethra. The other is transurethral incision of the prostate (TUIP), which involves cutting away diseased areas with an instrument inserted through a tube in the urethra.
In TURP, fluid from the bladder is drained out before surgery to make room for instruments. During the procedure, surgeons remove a portion of the prostate and then replace it with gauze to prevent bleeding. Afterward, this gauze is removed and replaced with stitches made from surgical thread.
In TUIP, surgeons cut away diseased areas using an instrument called a resectoscope that’s inserted through a tube in your urethra. This procedure takes longer than TURP because it requires more work to remove all diseased tissue. But because there’s no need to drain fluid from your bladder prior to surgery, there may be less pain afterward and less blood loss during surgery compared with TURP