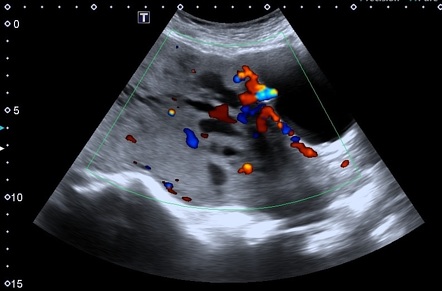
Placenta Accreta Ultrasound; To diagnose placenta accreta and determine the extent of placental invasion, an ultrasound and/or an MRI may be performed.
Ultrasound
Ultrasound can detect the presence of accreta by the following criteria:
absence of a normal decidua basalis overlying the myometrium on a transverse section,
presence of retroplacental echogenic bands,
absence of retroplacental blood flow on Doppler imaging, and/or
abnormal placental vascularity on color Doppler imaging.
These criteria have been shown to have sensitivities as high as 87% for diagnosing placenta accreta (SACOG, 2017). However, these findings are not specific for placenta accreta, and an ultrasound with equivocal findings in one or more areas does not rule out this diagnosis. In addition, the absence of these findings does not rule out the diagnosis. An ultrasound with confirmatory findings allows for appropriate planning for care during delivery and can help avoid complications from an unexpected diagnosis at delivery.
With placenta accreta, the placenta attaches itself too deeply and firmly into the uterine wall, which makes it impossible for it to separate naturally from the uterus after delivery. In rare cases, the placenta can even attach itself to other organs such as the bladder.
This is a serious condition that can cause excessive bleeding after delivery. The bleeding may occur both during and after delivery, and could be life-threatening for the mother if not treated promptly.
It is important to keep in mind that a regular ultrasound may not necessarily detect or diagnose this condition. A very experienced sonographer may be able to spot this in advance, but otherwise a special test known as an MRI (magnetic resonance imaging) scan is required to confirm the diagnosis.
Placenta accreta is commonly diagnosed during week 20 of pregnancy or later. It is most commonly seen in women who have had at least one previous C-section surgery, because the scar tissue from such surgeries acts as an ‘anchor’ that prevents the placenta from separating properly.
If you have been diagnosed with placenta accreta during your pregnancy, your healthcare provider will closely monitor and manage your condition until you deliver. If you are pregnant with twins or more babies
Placenta accreta is a serious obstetric complication that occurs when the placenta attaches abnormally to the myometrium. It is associated with prematurity, fetal growth restriction, postpartum hemorrhage, maternal mortality, and stillbirth.
The diagnosis of placenta accreta is made based on ultrasound findings of placental invasion into the uterine wall. The accuracy of ultrasound in diagnosing placenta accreta is unknown. To evaluate the accuracy of ultrasound in the diagnosis of placenta accreta.
We searched MEDLINE (1966-2007), EMBASE (1985-2007), CINAHL (1982-2007), and the Cochrane Library (Issue 1, 2007) for studies comparing fetal ultrasound with histopathology as reference standard for diagnosing placenta accreta. We also reviewed reference lists and contacted experts in the field to locate relevant studies.
Two reviewers independently selected studies for inclusion and assessed study quality using a modified QUADAS tool. Disagreements were resolved by consensus or through discussion with a third reviewer.
We identified 11 studies involving 160 women with placenta accreta diagnosed by histopathology and 184 controls without placenta accreta who underwent fetal ultrasound
Placenta accreta is a condition that occurs when the placenta attaches too deeply into the uterine wall. It can be diagnosed by ultrasound.
Normally the placenta attaches to the uterine wall, but in cases of placenta accreta, the placenta invades and is inseparable from the myometrium (middle layer of the uterus). This can lead to significant bleeding at time of delivery.
The majority of cases of placenta accreta occur in patients who have had a prior cesarean section. This is because placenta accreta typically occurs where scar tissue has formed from previous surgery in the uterus.
There are three different types of placenta accreta:
Placenta accreta: The placental tissue attaches directly over scar tissue from prior cesarean section or from other causes.
Placenta increta: The placental tissue penetrates into the uterine muscle.
Placenta percreta: The placental tissue penetrates through the entire uterine muscle into surrounding tissues such as bladder or bowel
Placenta previa and accreta are serious complications of pregnancy. Placenta previa is a condition in which the placenta attaches itself to the lower part of the uterus, close to or covering the cervix, and can result in heavy bleeding during delivery. Placenta accreta is a potentially life-threatening condition in which parts of the placenta dig deeply into the wall of the uterus and do not separate from the uterus after delivery. The higher the placenta is implanted (closer to the top of the uterus), there is more chance that significant bleeding will occur during delivery.
Diagnosis
Placenta accreta can sometimes be diagnosed with ultrasound imaging, but other modalities are needed as well. MRI is recommended for women suspected of having placenta accreta due to previous cesarean deliveries. The diagnosis often cannot be made until labor begins, at which time blood transfusions may become necessary if there is heavy bleeding.
The placenta is the organ that develops in your uterus during pregnancy. It provides oxygen and nutrients to your growing baby and removes waste products from your baby’s blood.
The placenta attaches to the wall of your uterus, and your baby’s umbilical cord arises from it.
Normally, after delivery, the placenta will leave your body within about 30 minutes. The medical term for this process is placental expulsion.
Sometimes, the placenta doesn’t separate from your uterine wall as it should, either partially or completely. This condition is known as an abnormally invasive placenta (placenta accreta).
How is Placenta Accreta Ultrasound Diagnosed?
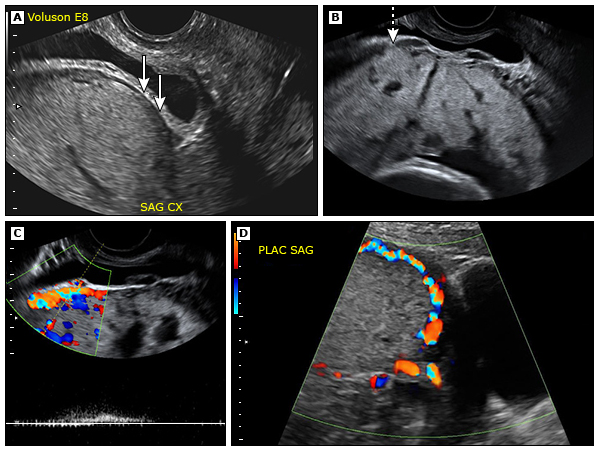
Ultrasound is the best way to diagnose placenta accreta. However, ultrasound has limitations, including:
It may be difficult to diagnose placenta accreta in its earliest stages.
Ultrasound can’t distinguish between an abnormally adherent placenta and a normal placenta with a retroplacental clot (blood clot behind the placenta).
The thickness of the lower uterine segment is measured to assess the risk of placenta accreta. Ultrasound measurements may not always be accurate.
The baby’s position can make it difficult to see the entire uterus on ultrasound.
Ultrasound is less reliable when performed by inexperienced ultrasonographers.
Doctors diagnose placenta accreta during an ultrasound. However, the condition may not be obvious in the early stages of pregnancy.
If you have risk factors for placenta accreta, your doctor may order a more detailed ultrasound later in pregnancy to look more closely at how the placenta attaches to the uterus.
In rare cases, doctors can detect placenta accreta by injecting dye into the uterus and then taking an X-ray (hysterography). The dye highlights any abnormalities in the attachment of the placenta to the uterine wall.
If your doctor suspects placenta accreta, they’ll likely refer you to a center with experience in managing high-risk pregnancies.
When placenta accreta is suspected, a special ultrasound is done. This ultrasound can diagnose the condition in 90 percent of cases.
In the remaining 10 percent of cases, the diagnosis is confirmed during surgery that is done for another reason. If you have had a cesarean section or another procedure to remove the placenta, your doctor might suspect placenta accreta if it was difficult to remove the placenta.
Placenta accreta is diagnosed by ultrasound. With placenta accreta, the placenta attaches itself deep into the uterus and in some cases grows into the muscles of the uterus.
With placenta accreta, the uterine wall will appear to be very thin because there’s not much blood between the placenta and the uterine wall. The ultrasound will also show a very dark circle around the edge of the placenta, which indicates that it is firmly attached to the uterine wall.
Most cases of placenta accreta are diagnosed before delivery by ultrasound. When the doctor suspects this condition, a more thorough ultrasound may be ordered. During the test, the doctor will look at the placenta and uterine wall to see if they appear to be attached. If so, the patient may be advised to have a C-section and possibly a hysterectomy.
Women who have had previous cesarean deliveries or a history of placenta accreta, increta, or percreta have a higher risk for having this problem again during subsequent pregnancies. These women should talk with their doctors about their options for birth control after delivery.
A doctor can diagnose placenta accreta by using ultrasound. An ultrasound is a test that uses sound waves to create images of parts of the body. It can show if the placenta is attached too deep in the uterus.
If you have a high-risk pregnancy, your doctor may order an ultrasound at your mid-pregnancy checkup around 20 weeks. If you have had a previous cesarean delivery and the placenta was low on the uterus, your doctor may order another ultrasound during this pregnancy.
Placenta accreta isn’t always detected by ultrasound. If there’s any doubt about whether it’s present, your doctor will use magnetic resonance imaging (MRI) to check for it. MRI uses magnets and radio waves to produce images of inside the body.
An ultrasound can show whether a placenta is attached too deeply into the uterine wall and whether blood vessels in the uterine wall have grown into the placenta.
Other tests that may be used include:
Blood tests. A mother may have anemia, low platelet count or other problems with her blood if she has placenta accreta.
A separate test called a hematocrit measures how much of your blood is made up of red blood cells (RBCs).
Hemoglobin test. This measures how much oxygen your red blood cells carry from your lungs to the rest of your body.
Platelet count. Platelets help your blood clot, so if you don’t have enough of them, you start to bruise and bleed easily.
Does Placenta Accreta Show On Ultrasound?
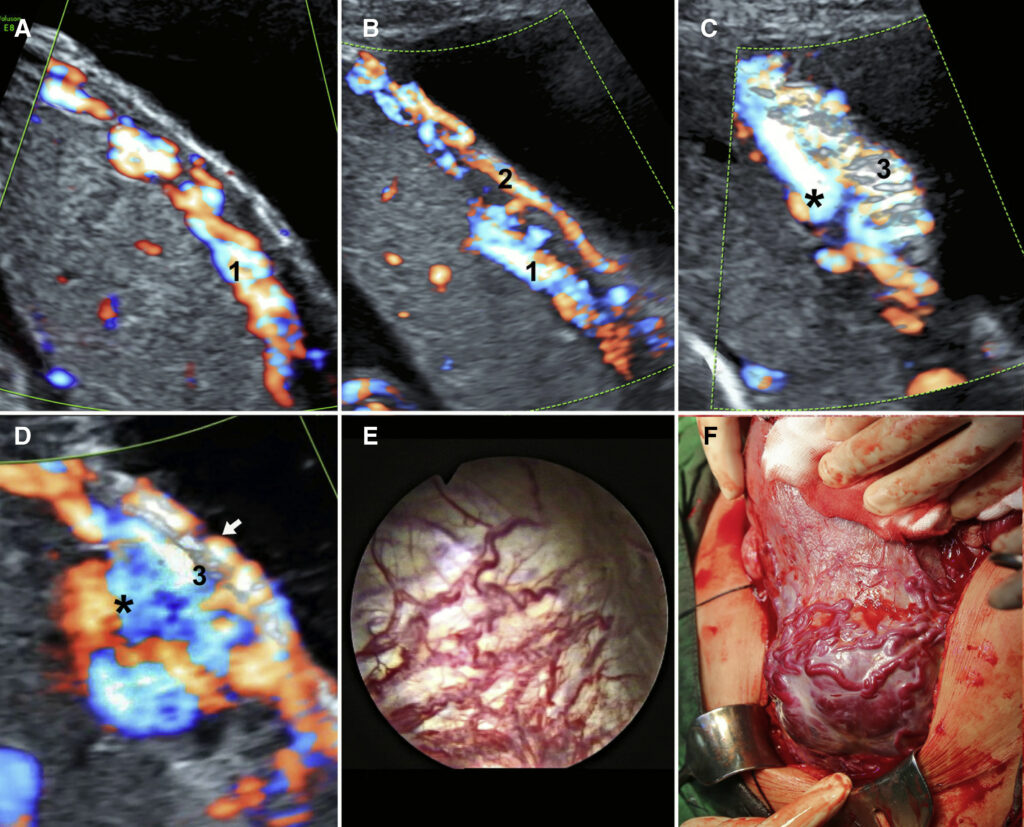
I just found out that I have placenta accreta. I had an ultrasound at 20 weeks, and the ultrasound tech said that everything looked great. I even asked her if she saw anything that looked abnormal and she said no.
Is it possible that placenta accreta could have been missed on my scan?
Answer:
Placenta accreta is a condition in which the placenta attaches too deeply into the uterine wall, sometimes into the muscle of the uterine wall (placenta increta) or even piercing through the uterine wall (placenta percreta).
Most cases of placenta accreta are diagnosed during the pregnancy, usually after about 20 weeks gestation using ultrasound scans. A few cases are not diagnosed until delivery, and some cases are never diagnosed.
An ultrasound technician may notice signs of placenta accreta when looking at an ultrasound image during pregnancy. However, it can be difficult for them to determine whether or not there is a risk for placenta accreta until later in the second trimester or early third trimester when enough information is visible on an ultrasound scan to make a diagnosis.
It’s also important to remember that not all cases of
Ultrasound is a valuable tool in the diagnosis of placenta accreta. In fact, it can often be suspected on ultrasound before delivery.
When the ultrasound is performed by an experienced operator, it may suggest the possibility of placenta accreta by finding:
Placental lacunae (cystic spaces)
Intrauterine blood flow to the placenta
Thickened endometrium
Maternal vascularity of the placenta (the appearance of blood vessels in the placenta)
Well-trained ultrasound personnel may be able to detect a placenta accreta on ultrasound. However, it is often difficult to accurately identify this condition before delivery. If the sonographer suspects that you have an abnormally invasive placenta, your doctor may order additional testing such as a magnetic resonance imaging (MRI) scan or a computed tomography (CT) scan.
Placenta accreta is a serious condition that occurs when the placenta grows too deeply into the uterine wall. It can cause severe bleeding after delivery and sometimes requires a hysterectomy to stop the bleeding.
Research has shown that ultrasound is very accurate in diagnosing placenta accreta before birth, but it’s not 100 percent effective. The condition may also be hard to spot on ultrasound because it can look like other conditions, such as placental abruption (when the placenta separates from the uterine wall).
There are no specific symptoms of placenta accreta, but symptoms can include:
Vaginal bleeding during pregnancy
Abdominal pain during pregnancy
Placenta accreta is diagnosed with ultrasound and magnetic resonance imaging (MRI). Blood tests are used to confirm the diagnosis.
The placenta is a temporary organ that forms during pregnancy to deliver nutrients and oxygen to the fetus. Normally, it attaches to the uterine wall and after the baby is born, detaches from the wall and leaves the body.
In placenta accreta, the placenta fails to detach after birth. This can be life-threatening for both mother and baby.
The condition can occur during any pregnancy, but it’s more likely if you’ve had a previous cesarean section or uterine surgery, previous placentas that have attached too deeply into the uterine wall or have been in previous pregnancies with unexplained bleeding before week 20.
Doctors suspect placenta accreta based on a woman’s medical history and symptoms. Doctors usually can confirm a diagnosis with an ultrasound or magnetic resonance imaging (MRI).
The placenta is the organ that develops in pregnancy that nourishes the growing baby. Placenta accreta is a condition in which the placenta grows into the wall of the uterus and fails to separate from the uterus after delivery. The placenta can be attached too deeply into the uterine wall or it can grow through the entire wall. This condition usually requires surgical removal of the uterus (hysterectomy) to stop the bleeding.
The baby can be delivered by cesarean section, and then hysterectomy performed after delivery. Sometimes this is not possible due to excessive bleeding and hysterectomy has to be performed when the baby is still inside. In some cases, where there are life threatening circumstances, hysterectomy may even have to be performed before delivery of the baby, a procedure called peripartum hysterectomy.
This condition most commonly occurs in women who have had multiple prior cesarean deliveries or who have had other uterine surgeries such as dilation and curettage (D&C). It can also occur in women without these risk factors as well, although less commonly. The incidence of this condition has increased over time due to increased number of c
A placenta accreta is an abnormality of the placenta in which the placenta attaches too deeply into the uterine wall. When this happens, it can cause hemorrhaging after delivery and can also cause complications during delivery.
The term placenta accreta refers to any degree of abnormal invasion of the placenta into the wall of the uterus. It is caused by a failure of decidualization (the process that allows for normal separation of the placenta after the baby is delivered) in the area where the placenta normally attaches to the uterine wall. Placental tissue normally rests on top of this decidua layer, but with a placenta accreta, there is no decidua layer, so placental tissue invades further into or through the myometrium (muscle layer of the uterus).
Placenta accreta can be categorized as partial or total depending on how deeply it attaches to and penetrates through the myometrium. Placentas that only attach to or penetrate through part of the myometrium are classified as partial; those that attach to or penetrate through all layers are classified as total or complete placental accretas. Partial placental accret