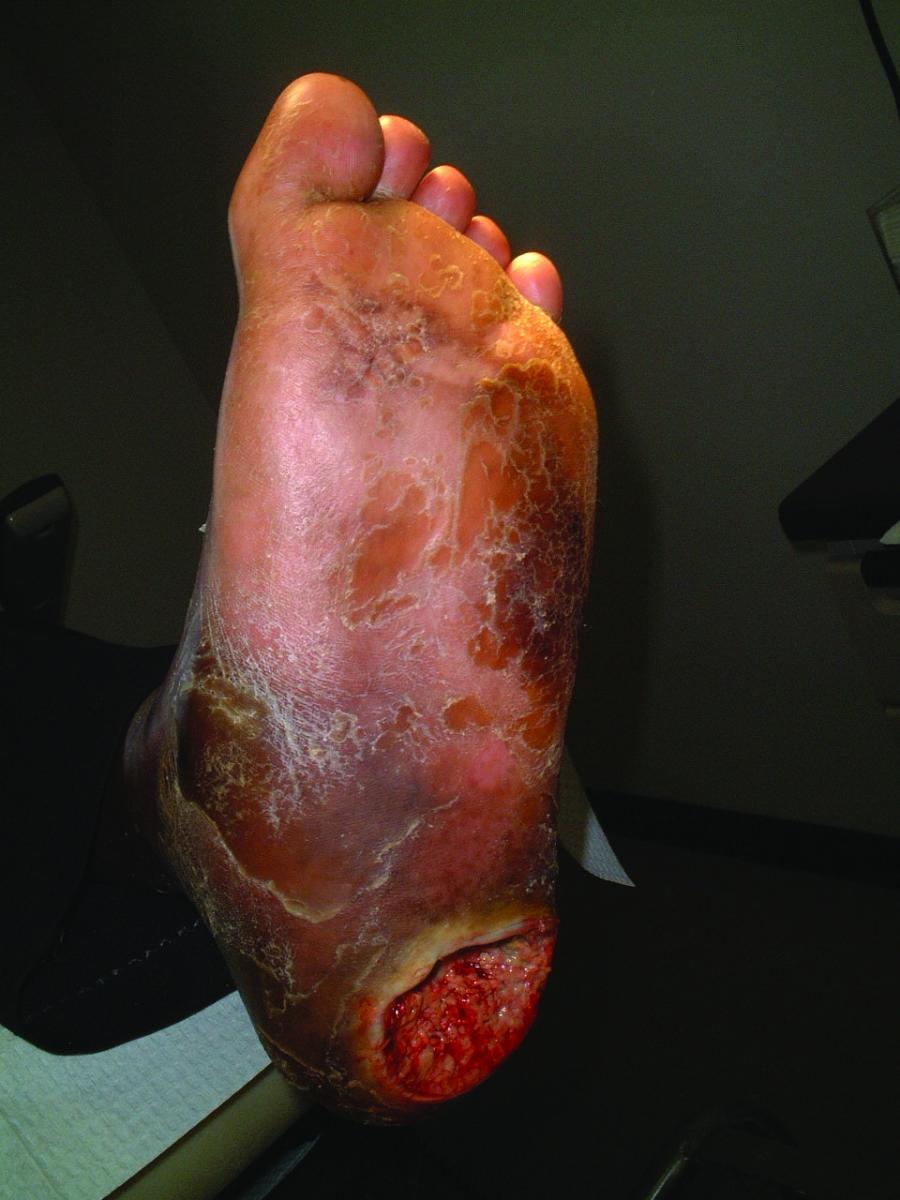
ICD-10 code for diabetic foot ulcer: L89.2
Diabetic foot ulcer is a condition in which there is damage to the feet due to a variety of reasons. The most common cause of diabetic foot ulcers is poor blood circulation in the feet. They are not only painful but also can lead to complications such as amputation of limbs or even death if not treated on time.
The ICD-10 code for diabetic foot ulcer is L94.9.
Diabetes is a disease that causes high levels of sugar to build up in the blood. Your body needs insulin, a hormone made by your pancreas, to convert sugar into energy. With diabetes, your pancreas does not make enough insulin or does not use insulin properly, so sugar cannot get into your cells. This causes you to have too much sugar in your blood. Over time, this can lead to serious health problems, including heart disease and kidney disease.
A foot ulcer is a sore on the bottom of your foot caused by damage to the skin over a bony area. Damage can be caused by an injury or by repeated rubbing against shoes or socks that are too tight. You may have more than one ulcer at a time.
What is the ICD-10 code for type 2 diabetes with foot ulcer?
The ICD-10 code for type 2 diabetes with foot ulcer is E08.
ICD-10 code for type 2 diabetes with foot ulcer is E09.0.
The ICD-10 code for type 2 diabetes with foot ulcer is E08.8.
This code is for use in situations where the patient has been diagnosed with both diabetes and a foot ulcer. The E08.8 code is only used in situations where it is not possible to determine which condition came first (the diabetes or the foot ulcer).
Type 2 diabetes mellitus with foot ulcer
E11.5 Diabetes mellitus, unspecified, with severe diabetic foot ulcer
E13.5 Diabetic neuropathy, unspecified, with severe diabetic foot ulcer
The ICD-10 code for type 2 diabetes with foot ulcer is E11.9.
The ICD-10 code for type 2 diabetes with foot ulcer is E08.
ICD-10 code E13.209
Type 2 diabetes with foot ulcer
ICD-10: E13.209 Type 2 diabetes with foot ulcer, unspecified limb
E13.209 is a type of diabetes mellitus, characterized by high blood sugar that can’t be controlled by diet alone. It’s caused by a lack of insulin (a hormone made by the pancreas) or the body’s inability to use insulin properly.
The symptoms of E13.209 include:
increased thirst, frequent urination and excessive eating (polydipsia, polyuria and polyphagia).
These symptoms may be followed by blurred vision, fatigue and weight loss (cachexia).
There is a code for this in ICD-10. The code is W56, which means:
W56 Type 2 diabetes mellitus with foot ulcer
This is one of the commonest causes of ulcers in diabetics.
You can find more information here: https://www.icd10dataonline.com/w56
What is the ICD-10 code for foot ulcer?

The ICD-10 code for foot ulcer is L54.8. This code is a non-specific code, which means that it does not describe the cause of the injury or condition. It is simply used to identify it and be able to track the progress of treatment.
The ICD-10 codes are based on the patient’s diagnosis, which can be any number of things: a particular type of cancer, an infection or other health problem, etc.
The ICD-10 code for foot ulcer is T33. The ICD-10 code T33 stands for “ulcer of skin and subcutaneous tissue of toe, foot and heel”.
The ICD-10-CM is the International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Clinical Modification, which is a diagnostic classification system published by the World Health Organization (WHO). It contains codes for all health conditions. The ICD-10 code T33 also has corresponding SNOMED codes.
ICD-10 Code for Foot ulcer: S31.0 – S31.9, M85
The International Statistical Classification of Diseases and Related Health Problems (ICD) is an international classification that contains codes for health conditions and their causes. The ICD is published by the World Health Organization (WHO). The ICD-10 is the 10th version of the ICD, first published in 1990 by WHO.
How do you classify a diabetic foot ulcer?
The treatment of diabetic foot ulcers is challenging and complex, with many factors that can affect treatment. The most important factor is the location of the ulcer.
Superficial foot wounds are the most common type of ulcer, and these wounds are usually managed with conservative measures such as dressings or oral antibiotics. Deep foot wounds require surgical intervention to remove dead tissue and restore blood flow to the area.
The classification system for diabetic foot ulcers was developed by researchers at the University of Pittsburgh School of Medicine, who published their findings in The Journal of Bone & Joint Surgery in 1997. They found that there were two types of chronic foot wounds: superficial infections and deep necrosis. Superficial infections were characterized by redness around the wound, while deep necrosis showed no signs of inflammation but had poor circulation due to poor vascularization (poor blood supply).
A diabetic foot ulcer is an area of skin that has been damaged by a lack of blood supply. The skin may look pale and dead because it is not receiving enough oxygen.
A diabetic foot ulcer can be classified as:
Superficial foot ulcer — This is the most common type of diabetic foot ulcer. It occurs where the skin meets the sole of your foot, for example near your big toe or heel. A superficial foot ulcer usually heals well with good treatment.
Deep foot ulcer — Deep foot ulcers are more serious than superficial ones, because they affect deeper layers of skin and tissue below the surface of your skin. Your doctor may need to remove dead tissue from a deep foot ulcer before it can heal properly.
What Is a Stage 2 diabetic ulcer?
The stages of diabetic foot ulcers are based on their depth. Stage 2 is the most serious stage and requires immediate treatment.
Stage 2 diabetic ulcers are deep wounds that have penetrated all layers of skin, including the muscle and bone. The skin has turned black or gray, and you may see bone. The wound is usually painful, but you may not notice it if you are diabetic because nerve damage associated with diabetes can make you insensitive to pain.
A Stage 2 diabetic ulcer needs immediate treatment for several reasons:
The wound can become infected and may spread to other parts of your body if left untreated.
If you have poor circulation in your legs or feet, blood clots could form in your veins and travel to your lungs (pulmonary embolism). This is a life-threatening condition that requires immediate medical attention if it occurs.
Diabetic ulcers are some of the most common foot problems that people with diabetes have to deal with. They can be caused by poor circulation, which can lead to sensory nerve damage. Diabetic ulcers often take weeks or even months to heal and sometimes require surgery or skin grafts.
What Is a Stage 2 diabetic ulcer?
A stage 2 diabetic ulcer is when the tissue under the skin starts dying because of poor blood flow to the area. This causes redness, pain and swelling. If this continues for a long period of time, it can lead to an infection in your skin.
What is a Stage 3 diabetic ulcer?
A Stage 3 diabetic ulcer is a poorly healing ulcer that has penetrated to the muscle.
Stage 3 diabetic ulcers are very serious and can lead to amputation of toes, feet or legs if left untreated.
Some people with diabetes have one or more deep foot ulcers that do not heal within 2 weeks of treatment. A Stage 3 foot ulcer is also called an unhealing foot ulcer. These wounds usually develop on the bottom of the heel or on the ball of the foot and may look like large blisters filled with blood.
Diabetic foot ulcers develop when nerve damage prevents a person from feeling pain in their feet and legs. This makes it hard for them to notice when they have an injury or wound on their feet. If you have diabetes, you should see your doctor right away if you notice any sores on your feet that don’t heal within 2 weeks of treatment
A stage 3 diabetic ulcer is a wound that has become seriously infected, and the damage can be extensive. It can take several weeks or months to heal, and it may require surgery.
The main symptom of a stage 3 diabetic ulcer is pain and swelling. You may also have redness, warmth, or tenderness around the area.
A stage 3 diabetic ulcer usually affects your feet. You may have other symptoms such as:
redness, swelling or tenderness in your toes or feet
a burning sensation when you walk
a feeling of weakness in your legs
How do you classify pressure ulcers?

There are several types of pressure ulcers, each with its own characteristics and treatment strategies. The most common type of pressure ulcer is the decubitus ulcer, which is also known as a bed sore or pressure sore.
Pressure sores are classified by their location and depth. They can range from mild to severe and are described in terms of stage:
Stage 1: A red or blanched area of skin that may be painful, but doesn’t show scale or other signs of damage. The area is generally firm to touch, but there may be a loss of firmness at the edges.
Stage 2: A reddened area that’s covered by superficial wounds and has some scaling, dryness and possible hemorrhaging. There may also be some swelling around the wound.
Stage 3: A breakdown in tissue through dead tissue into underlying muscle or bone in an advanced stage of healing that causes a pocket effect where fluid collects under the skin’s surface (seroma). This stage indicates that infection may have occurred.
There are three main types of pressure ulcers.
Stage 1: A stage 1 pressure ulcer is reddened skin that’s caused by pressure and friction. It doesn’t penetrate far into the skin.
Stage 2: A stage 2 pressure ulcer is already healing, with a shallow crater or pocket of dead tissue beneath the skin’s surface. The crater is an inch or less in diameter.
Stage 3: A stage 3 pressure ulcer goes all the way through the skin’s surface and down to the underlying tissue (muscle, bone or fat). It may be deep, but it’s not wide enough to expose underlying structures like tendons or bones.#ENDWRITE
How do you grade an ulcer?
There are several grading systems for ulcers. The most common one is the Ulcer Clinical Activity Index (UCAS), which grades the size and depth of an ulcer.
The UCAS scale goes from 0 to 24, with higher numbers reflecting greater severity. The score is based on three factors:
Depth (1-3) — This refers to how deep the ulcer is, measured in millimeters. A 1-mm-deep ulcer is more superficial than a 5-mm-deep ulcer.
Size (1-5) — This refers to how large the ulcer is, measured in centimeters squared. A 1-cm2 ulcer is smaller than a 10-cm2 ulcer.
Erythema (1-4) — This refers to how red or pink an area around an ulcer looks, measured in millimeters squared. A small area of redness around a 2 mm deep by 2 cm2 sized ulcer would receive a score of 4 because it’s much larger than just being red or pink skin around the site of injury
Ulcers are graded based on the depth of the ulcer crater. In general, an ulcer crater that is less than 50% of the thickness of the skin is considered a Stage 1 ulcer. A Stage 2 ulcer crater is greater than 50% but less than 75% of the thickness of the skin. A Stage 3 ulcer crater is greater than 75% of the thickness of the skin and extends down into subcutaneous fat tissue.
Stage 4 ulcers are deep enough to penetrate through all layers of skin and enter muscle or bone, which are called neuropathic ulcers.
What is a grade 3 wound?
Grade 3 wounds are severe, deep wounds that involve the muscle and/or bone. These wounds are caused by high-energy trauma such as gunshots, knife wounds, or other sharp objects. They require immediate medical attention because of their serious nature.
Grade 1, 2 and 3: Wound categories explained
A grade 1 wound is a shallow cut or abrasion that only involves the top layer of skin (epidermis). It will heal on its own within days without any need for special treatment.
A grade 2 wound is a deeper cut that extends into the dermis (the second layer of the skin). These wounds may take up to two weeks to heal without proper treatment but can be healed completely if treated properly.
A grade 3 wound is a deep wound that extends into the subcutaneous tissue (third layer) or deeper into muscle or bone tissue; they require immediate medical attention because they can be life-threatening if left untreated.
A grade 3 wound is the most serious type of wound. It’s caused by a deep cut or puncture that reaches into the muscle or bone underneath. You may need surgery to repair such wounds, and even then you could be left with permanent loss of use of the limb.
The cause of a grade 3 wound is usually severe trauma, such as being hit by a car or falling from a height onto concrete. If you’re involved in an accident and have a grade 3 wound, seek emergency medical care immediately.
What is a Stage 3 foot ulcer?

Stage 3 foot ulcers are the most serious type of foot ulcer and require urgent attention.
Stage 3 foot ulcers are usually caused by peripheral arterial disease (PAD), a condition where arteries become narrowed and damaged, which can lead to ulcers and amputations. These ulcers tend to be larger and deeper than Stage 2 foot ulcers, so they will take longer to heal.
The main way to treat Stage 3 foot ulcers is through surgical intervention. This can involve bypass surgery or grafting, where a piece of vein or artery is used to bypass the blocked arteries in order to improve blood flow. If this isn’t possible, then a toe or partial foot amputation may be required.
A Stage 3 foot ulcer is a wound that has progressed to the point where it is not healing as well as it should.
An ulcer is an open sore or wound on the skin that does not heal after about three months. The length of time needed for a wound to heal varies depending on the type of ulcer and whether it is infected. Some wounds take months or even years to heal completely.
A Stage 3 foot ulcer is an advanced stage of a diabetic foot ulcer, but it may also be caused by other conditions or diseases that damage or destroy soft tissue.
A Stage 3 foot ulcer is an advanced stage of a diabetic foot ulcer. It is characterized by:
Exposure of the bone or tendon
Infection in the bone or tendon
Extensive tissue necrosis (death)
A Stage 3 foot ulcer can be painful and will not heal without surgical intervention. A Stage 3 foot ulcer requires immediate medical attention and treatment.